News & Events
BPA in the News
Financial Literacy Creates a Better Future

Written by Z.D.
The COVID-19 pandemic began earlier this year as a public health crisis, but quickly morphed into a mental health and economic crisis. Events caused by the pandemic – employees working from home, furloughed, laid off or forced to work on the front lines – pulled back the curtain on the lack of financial preparedness many Americans are facing.
In April, unemployment rates reached the highest level since the Great Depression. As a result, claims for unemployment benefits rose dramatically. However, millions of people who lost their jobs were unable to apply for this benefit. Still, these figures do not reveal the extent to which American families are struggling financially as a result of COVID-19-related job loss.
Read the full article in Building Trades News' October issue.
What to Know Before Open Enrollment

Source: Z.D.
While few things have remained certain in 2020, one event that will continue as planned is open enrollment — the period when you’re able to change your health plan for the upcoming year.
Timelines vary, but most HR departments hold open enrollment for a few weeks between October and December. During your open enrollment period, you’re able to select your health care coverage for Jan. 1 through Dec. 31, 2021. If you miss the deadline, you’ll typically remain with your current health plan until next year’s open enrollment period — that is, unless you change jobs or have what’s known as a qualifying life event, such as getting married or having a child.
While it might feel overwhelming, the choice you make can have a big impact not only on your health, but on your finances as well. Here’s what to know before open enrollment so you can make the decision that’s right for you and your family.
Read the full article on Northwestern Mutual.
Differences Between a Furlough and a Layoff

Source: Z.D.
Downsizing your company is never easy, especially in times of financial hardship. Employee salaries are one of the highest overhead costs for businesses, though, so furloughing or laying off employees may be your best (or only) option in a financial crisis. Before going down this path, you should understand the differences between furloughs and layoffs to determine which is the better solution for your business.
Read the full article on Business News Daily.
Learn the differences between FSAs, HRAs and HSAs to determine which is best for your business.

Source: Z.D.
When you're creating a competitive benefits plan for employees, good healthcare options should be a top priority. In addition to health, dental and vision insurance, many employers choose to offer employees supplemental tax-free accounts that can be used to pay for medical costs, such as flexible spending accounts (FSA), health reimbursement accounts (HRA) and health savings accounts (HSA). Although the purposes of these accounts are similar, there are a few key distinctions that will determine which one is right for your company.
Read the full article on Business News Daily.
The Power of Organized Labor

Written by Z.D.
This year, more than ever, it is important to celebrate Labor Day. This holiday pays tribute to the contributions and ingenuity of American workers. While it traces its origins to well before the Industrial Revolution, organized labor and unions are as relevant and necessary as ever before, constantly adjusting to new challenges and in recent times, facing down the odds with renewed resolve. It is worth asking whether the systematic erosion of organized labor seen these last 25 years, and its undoubted erosion of communal society, has left us in a weaker position as we battle against COVID-19.
Labor unions have been part of the American landscape since the nation’s founding, with the formation of the Federal Society of Journeymen Cordwainers (Shoemakers) as early as 1794 in Philadelphia. However, much of the serious work of organized labor came into effect after the Civil War, with the National Labor Union formed in 1866 precisely to convince Congress that the number of hours worked in a week needed regulation. As industries changed from household craftsmen to mechanized factories, the market expanded beyond local boundaries and new levels of supply and demand determined an expanding economy.
Read the full article on Building Trades News: Labor Day Issue.
An Update on COVID-19 Assistance: Presidential Executive Orders

Recently, President Trump signed one executive order and three executive memoranda with the promise to provide additional assistance to Americans hurting financially from the COVID-19 pandemic. But from halting evictions to pausing payroll taxes and providing additional unemployment benefits, what do these executive actions accomplish?
A $400 Unemployment Benefit
Under the recent executive memorandum, the federal government would contribute $300 of the $400 payment allocated. This is down from the $600 allocated in the CARES Act passed in March, which ended July 31. Individual states, already under financial stress due to the coronavirus outbreak, are responsible for the remaining $100 per person per week, retroactively starting Aug. 1.
Eviction Bans and Relief
The executive order leaves the decision to ban evictions to Health and Human Services Secretary Alex Azar and Centers for Disease Control and Prevention Director Robert Redfield, taking no official stance itself. It also doesn't say if it will provide financial assistance to renters, leaving that decision to Mnuchin and Housing and Urban Development Secretary Ben Carson.
Student Loan Deferral Extension
The White House's memorandum on student loan deferral moves to waive student loan interest until December 31, extending current relief under the CARES Act that is set to expire September 30 by two months. Payments are scheduled to restart on January 1, 2021. The executive memorandum applies to loans "held by the Department of Education," which doesn't include privately held student loans, such as through a bank.
So far, the executive actions will cover only the four topics above, rather than the large scope of either party’s stimulus proposals negotiated in Congress. The executive orders are also not bills signed into law and can only do so much on their own. The executive orders did not address the following:
- • Testing, tracing and treatment of COVID-19
- • Money needed to safely reopen schools and provide personal protective equipment
- • Food assistance
- • Aid for local and state governments
- • Money ensuring that elections can be safely carried out
- • Money to keep post offices open for elections
Both parties note that it is possible for talks of COVID-19 relief legislation continuing. If talks resume, stimulus legislation could come to a vote in one chamber later this month, but both chambers must vote before the legislation goes to the White House for the president’s signature. If a deal is reached in the coming weeks, it's also possible that the executive actions will be null and void.
As negotiations continue in Washington, BPA will continue to monitor developments and provide updates to our members. Stay tuned to our website for more details.
CARES Act Benefit Assistance

The Coronavirus Aid, Relief, and Economic Security Act (the CARES Act) authorizes more than $2 trillion to battle COVID-19 and its economic effects, including immediate cash relief for individual citizens, loan programs for small business, support for hospitals and other medical providers, and various types of economic relief for impacted businesses and industries.
Many benefits remain available through the end of the year and beyond to mitigate the impact felt by the pandemic, while negotiations are still in the works to provide extension of relief, such as the federal unemployment benefit. Check with your state to learn more about potential changes to state unemployment benefits.
Below is a roundup of benefits still available to both employees and employers via the CARES Act:
Student Loans
All payments of principal and interest for certain federal student loans are suspended. The suspended payments are treated as if made for consumer credit reporting. The CARES Act also waives or modifies requirements with respect to the receipt of federal education grants, and allows deviations in the use and distribution of such grants. Further, provisions are made for students who have withdrawn from school or relocated due to the COVID-19 crisis.
Student Loan Repayment-Employee Education Assistance Program
Employers may provide a student loan repayment benefit to employees on a tax-free basis of up to $5,250 annually towards an employee’s student loans. The cap takes into account both any new student loan repayment benefit as well as other educational assistance currently provided by the employer. The provision applies to any student loan payments made by an employer on behalf of an employee after March 27, 2020, and before January 1, 2021.
Retirement Plan Relief
The CARES Act provides for additional relief for individuals with respect to distributions and participant loans under defined contribution plans. More detail is provided below under the heading Retirement and Other Employee Benefit Plans Relief.
Federally Backed Mortgages
Borrowers under federally backed family mortgages may submit a forbearance request if they are experiencing financial hardship due to the COVID-19 crisis. The lender must grant the request, without penalties, fees or interest, for a period of up to 180 days (subject to another 180-day extension at borrower’s request). Foreclosure action is prohibited for the 60-day period beginning March 18, 2020. Multi-family borrowers (assets designed for occupancy of 5 or more families) are entitled to forbearance and foreclosure protection on slightly different terms, and renters of such dwellings are provided eviction protection.
Retirement and Other Employee Benefit Plans Relief
The CARES Act provides additional relief with respect to distributions and participant loans under defined contribution plans, funding relief for defined benefit plans and enhanced flexibility for health care options and tuition assistance. The deadline for amending retirement plans for these changes is the last day of the first plan year beginning on or after January 1, 2022. These provisions can be implemented immediately. What this means to you is that these provisions offer employees and employers additional options to address the potential financial hardships that arise as a result of the effects of COVID-19 and offer additional ways to access health care and prescriptions.
Minimum Required Distributions
The CARES Act temporarily waives the required minimum distribution rules for 2020 with respect to certain defined contribution plans and IRAs.
Coronavirus-Related Distributions
Individuals may take coronavirus-related distributions from qualified retirement plans of up to $100,000 without such distributions being subject to the 10% early distribution tax. Such distributions are subject to federal income taxation, which may be ratably spread over the three taxable year period beginning with 2020. An individual who takes a coronavirus-related distribution may repay the distribution to an eligible retirement plan during the three-year period beginning on the day after the date of the distribution. Repayments within the three-year period will result in the distribution not being subject to federal income taxation, or in the case that the income tax has already been paid, permit the individual to receive a refund of the previously paid federal income tax. An individual must satisfy certain requirements in order to qualify for coronavirus-related distributions.
Funding Relief for Defined Benefit Plans
Any required minimum contributions for a single employer defined benefit that are due during the 2020 calendar year are not required to be made until January 1, 2021, with accrued interest from the original payment due date to the actual payment date. Additionally, plan sponsors of defined benefit plans may treat the last plan year's adjusted funded target attainment percentage as the percentage applicable to plan years which include the 2020 calendar year for purposes of applying the funding-based limitation on shutdown benefits and other unpredictable contingent event benefits.
BPA continues to monitor the evolving situation with COVID-19 and will provide updates as they become available.
Essential Services for Essential Times

Written by Z.D.
The COVID-19 crisis has forced the adaptation of almost every industry and the transformation of millions of lives in the course of a few weeks. For some individuals, this change occured in the course of a single day. Lives were upended, regulations changed, and systems have been altered. However, advances in technology have allowed businesses to stay connected, maintain operations, and ensure the livlihood of the millions of customers they serve.
Remote work simply wasn't considered a viable option, especially in the benefits industry environment; however, the wider use of technological advancements has made the transition to a work environment broadly accessible from the remotest parts of the globe. Software systems allow secure access to documents and empower collaborative workforces. Communication, project management and time traking softward continue to grow smarter and keep teams connected while miles apart. Industries that were largely in-person, due to the sensitive nature of operations, now have the ability to confidently and confidentially conduct business in a manner that protects clients while ensuring business advancement.
Read the full article on HR.com
Employee benefits shouldn't just look good on a PR blurb. Here are the benefits that add value to your employees' lives.

It is important for companies to offer benefits and perks that attract, retain and impress employees. Zane Dalal, executive vice president of the Benefits Programs Administration, spoke with Business.com about finding benefits that add true value to your employees' lives.
The most important thing to do, he said, is to listen to your employees.
"I cannot stress this enough," he said. "Send out an officewide survey. Take down notes and suggestions from an all-staff meeting. Hearing directly from your employees is key when developing or redeveloping any benefits packages in the workplace."
Read the full story.
BPA Encourages Workplace Mental Health - Building Trade News

It’s no secret that a productive work environment stems from happy employees. For most Americans, a large part of their daily lives is spent at work. According to the Mental Health America advocacy group, less than one third of Americans are happy with their work. Not only does this decrease productivity from employees, but it also puts employees’ long-term mental health at risk. In order to improve productivity in your business, there must be an awareness and understanding of the workplace environment and how it can be adapted to promote better mental health for employees.
Read the full story.
How Technology is Shaping the Benefits Industry - February 28, 2020

For Employees
Online Employee Benefit Portals. These online portals are providing open communication and access for all benefits related questions. Information on current company policies, benefit forms, newsletters and all benefit related news exist in one place so employees can sort through them privately and securely at their own convenience. Benefits portals can also include sections for health care and financial literacy, a medical reference library or online health care advice.
Virtual Health Care. As society figures out new ways to reach people in remote locations and provide the best care to individuals across the country, no matter where they live, virtual health care is taking off. This benefit provides a tool for employees to have access to medical care in non-emergency situations, without having to visit a doctor in person. Conducting consultations via app, online portal or video conference allows employees to use the latest technology to resolve medical concerns almost immediately.
Growth of AI. The recent rise of artificial intelligence across the benefits industry has resulted in more customized benefit plans for employees, as well as better customer service and more streamlined troubleshooting. Artificial intelligence can now provide recommendations based on prior history and employee preferences. This technology also allows benefits providers and administrators to offer the best customer service by carefully archiving notes from previous conversations with representatives for reference, offering a stress-free experience to employees.
Rise of Apps. Keeping employees engaged while promoting healthier lifestyles at the same time may be answered with the use apps. Promoting health information through apps at an employees’ fingertips has gained popularity over the last five years. These apps allow employees to track their own personal health progress, get additional, personalized information and help them make decisions about their health benefits based on their current health status. Apps that are game-based platforms can also be used to drive specific behaviors via competitions, where employees can score points, badges, etc. for achieving certain health or wellness goals (e.g. attending regular health check-ups or quitting cigarettes).
For Employers
Streamlined Employee Benefits Administration. Employee benefits administration is likely the main concern for most organizations. With the advancement of technology in the benefits industry, human resources and benefits administration teams can access all employee data, view and analyze claims, make updates to the insurance policies, and use the accounting section and direct billing to further streamline administrative tasks.
Online Enrollment Platforms. As technology has evolved in the benefits industry, providing open online enrollment to employees has allowed the employee themselves to take control of their enrollment, give them ample time to consider options and relieve human resources and benefits administrators of enrollment tasks. Online enrollment is tightly connected to employee benefits online portals, where new employees can use existing data or input new data themselves, compare insurance plan options, and they choose to extend it to their families, for example, they do not need to include human resources or benefits administrators in the process. Consider utilizing an online enrollment if it fits the needs of your organization.
Data Storage and Analysis. Cloud storing of data, as well as a backup, is always a great idea; storing data in the cloud is secure – and is just as cost effective as much as the traditional printed way. However, benefits administrators can use data to improve current employee benefits plans. Programs that help measure the effectiveness of benefits plans by analyzing claims data or spikes in turnover can help companies better understand how their staff is using benefits packages, and what changes should be done to include benefits that are most important to the employees.
Simply consider these new options in technology as they are the way employee habits are trending in other sectors. At the end of the day, each organization should do what is best for itself and its employees.
Technology-powered service is what sets BPA apart. Our online User Portals improve collaboration and communications among trustees, participants, and the benefits professionals that serve them. With the advancement of technology ni the benefits industry, we have been able to provide top-notch customer service and streamlined benefits administration to all of our customers. Contact us to see how we can help serve you today.
Read the full story.
Organized Labor Struggles in the American South

On January 28, BPA Executive Vice President Zane Dalal was featured in a UnionTrack piece, "Why Organized Labor Struggles in the American South." Zane offers that younger generations may hold the key to revitalization, "Millennials are incredibly adaptable, and people think of them as this sort of vague group, yet they are activists and they're incredibly sure of what they want."
Read the full story.
Are You Prepared for 2020?

Anticipating the shifting political landscape in 2020, Benefit Programs Administration (BPA) is tracking the latest policy developments in Washington. We understand that these policies touch each part of our industry in a unique way and are working to understand the implications to better serve our customers.
The upcoming 2020 presidential race is growing closer and candidates have their own ideas on how to protect retirement in America, address the student loan crisis and reform the health care system.
Many candidates are discussing Medicare for all, a system that concerns many union members. Medicare for all moves every person from private, employer-sponsored health insurance over to a single-payer system. While some unions support the single-payer legislation put forth by Senator Bernie Sanders (I-VT), others are not so enthusiastic. Quality health care plans negotiated between unions and employers are traditionally very good plans, and many union members enjoy them.
Additionally, some candidates are discussing cancelling student loan debt. While this may or may not become a reality, it changes how employers are recruiting new talents and the retention of existing talent. Employers who offer student loan repayment as a benefit may need to alter their plans to appeal to a younger generation with mounting student debt.
Changes to retirement and pensions could also be on the horizon in 2020. The Senate counterpart of the SECURE Act is RESA, The Retirement Enhancement and Savings Act, which was reintroduced in March and awaits a vote. The most notable provisions in RESA include automatic enrollment credit for small businesses where employers offset start-up costs for new 401(k) plans and SIMPLE IRA plans that include automatic enrollment and a unique component that would allow small businesses to band together and creat open mulitple employer plans (MEPs), rather than offering a plan alone or requiring a 'common bond' between employers as under current law.
State employee benefits like health insurance and PTO aren't going anywhere. However, there will likely be a shift toward more perks that impact employees' day-to-day lives. Student debt repayment, childcare, extended PTO, fertility treatments, pet health care, retirement planning, and gym membership plans are all examples of issues that employees tackle on a daily basis that employers have stepped in to help alleviate.
Companies are also turning to 'flashy' benefits and perks like unlimited snacks, daily yoga, and foosball tables over traditional employee benefits in an attempt to appeal to millennials and Gen Z workers entering the workforce. However, according to a survey by staffing firms Robert Half International, workers are partial to familiar staples like flexible work schedules (88%), bonuses (77%), and health insurance (69%), while amenitites like an on-site gym or child care (38%), or paid time off to colunterr (31%) draw less attention. MIT reports that, contrary to the stereotype, millennials and Generation Z are not more likely to be motivated by flashy perks than their older colleagues.
The administrators and staff at BPA work around the clock to track and understand the latest in benefits and employment policies. For more information on upcoming policy changes, benefits administration, or how you can work with BPA, please contact us. Be sure to chack out BPA Executive Vice President Zane Dalal's published article in HR.com about how HR professionals can prepare amidst policy uncertainty.
Happy Holidays from BPA Benefits

We at Benefit Programs Administration wish all our colleagues and friends a wonderful holiday season with a Merry Christmas and continued success in the coming New Year.
We cherish the long-lasting friendships we have been privileged to form, and we look forward to the new friendships that are yet to come.
From our BPA family to yours,
Happy Holidays!
Lili Gaspar: Don't Let Fear Stop You From Exploring Your Potential

I started my journey at BPA in the call center, answering phones for union representatives about benefits, eligibility and other related questions for participants. I traveled to open enrollments and provided support wherever it was needed. Then, during the early 2000s, we began growing very rapidly and the service demand was high, so my manager suggested I become a lead, which transpired into being call center manager, and then moving on to claims manager. I’ve been very fortunate to work on both sides of the third-party administrator process and I feel like it makes me a better administrator for clients.
This shift was a difficult transition at first -- starting as a peer to my coworkers and becoming a manager -- and I had to gain the trust and loyalty of the staff over time. That was such an important factor for me because gaining that trust would grow into loyalty. I’ve learned that when you build trust among those you manage; they are happier and more willing to meet and exceed expectations. In 2017, I became an assistant administrator as a supportive role for administrators and then shortly thereafter transitioned into an administrative role. With that transition, I learned more of the backend in benefits approval instead of the client-facing roles I had previously held. I strongly believe my experience with the plan participants gave me better insight on this side of my career.
BPA has given me these incredible experiences and opportunities, allowing me to grow both personally and professionally. I’ve been able to flourish in every direction, which has allowed me to try out courses in various areas of benefits administration, one in particular being claims. The mentorship and guidance I received while starting at BPA really went a long way and shaped me into becoming the best I knew I could be. Lance was a great mentor of mine when I first started at BPA and I’ve continued to follow his advice while growing within the company.
No matter what direction an employee wants to take, BPA really encourages them to explore those opportunities and reach for every goal. Before going out to the general public to find an individual to fill an open position, they’ll look in house to see if someone within BPA is a better fit. Everyone here gets the chance to explore their own potential.
Many women in the workplace don’t get the same opportunities. Some feel as though they need to blend in, do their job in the background, and avoid attention. That mindset can hold them back from reaching their true potential. It’s important that women within a company or industry, regardless of what that may be, speak up, express what’s on their mind and advocate for themselves. Confidence is key and advocacy for yourself and for other women will go a long way in creating change.
When it comes to growth or change, it’s crucial to seek out mentors who can help. Employers can foster this type of environment, striving to be a mentor and a coach to those they oversee by motivating employees to do better, teaching employees how they can improve and giving them more learning opportunities for everyone, not just women in their workplace.
Unions can and have been advocating for women in the workforce by giving them a platform to grow and build from. Women used to be a minority in the workforce and unions were a big part in opening the door. Many female-focused benefits became a more widely accepted policy in the non-union workplace once unions took those first leaps. The women’s movement, in particular, really brought family and maternity leave to the forefront as mainstream policies.
Today, it’s important we continue to push for workers’ rights and benefits including more time with families and newborn babies, men asking for more paternity leave, and so on. If it’s not you needing this extra time, it’s someone you know. People are very quick to assume “it’s only me,” or “I can’t do it” when it comes to creating change or making an impact. There is power in numbers, and there’s no better proof of that than seeing the achievements made by unions.
Building Trade News: Why a TPA is the Smart Way to Go

In this month's issue of Building Trades News, BPA Executive Vice President Zane Dalal highlights the benefits of partnering with a TPA.
Denise Wampler: "It's All About Balance" - November 20, 2019

Women comprise 47 percent of the U.S. workforce and have fueled 51 percent of the workforce growth in the past ten years. At BPA, we stand behind gender equality in the workplace and seek to elevate women into leadership and supervisory roles. We believe that when we allow a diversity of opinions at the table, our organization flourishes. BPA’s Women in the Workforce is a monthly blog series featuring female employees from the BPA team discussing their personal challenges and triumphs in the workplace. Each woman offers her own insight into how to overcome these challenges, how impactful the support of women can be and how employers can help combat the problem of inequality at work.
Working for BPA and the benefits industry in general is very gratifying. Helping people understand their healthcare and pension plans is very rewarding. It’s great to see them connect the dots, that the portion of their paycheck is taking care of their healthcare or contributing towards their future years. Unfortunately, younger people don’t realize that over time, their contributions add up. Some people who put aside a portion of their paycheck throughout the years, can retire quite well now.
In my opinion, the biggest challenge women face in the workplace is dropping the paradigm of the “carrot stick” management style – a combination of reward and punishment - it’s not working. Women bring connection, while men are very objective – it is a balance that is necessary to empower one another. In this industry, a nurturing and caring nature is important to communicate about the long-term effects of the benefit plans we administer. Quite of few of the ladies I work with the various departments (i.e. customer service and pension) have very nurturing personalities and able to put members at ease when they call incredibly worried.
Another area that women need to focus on is: working with each other instead of in competition with one other. By empowering supportive female relationships, there have been links to higher workplace happiness, lower rates of depression and lower employee turnover. The leadership at BPA is great at creating a collaborative environment and that is has been key to the longevity of our employees. The owners are mindful about promoting from within the ranks, thus allowing people with experience to lead the various division effectively.
My advice to other employers: Focus at your employees’ strengths and assist them to overcome their weaknesses. At BPA, the owners have been very good to provide tools for leadership growth, be it software, classes or training. Also, providing other incentives such as college tuition, leadership training is advantageous for keeping the employees working at their best.
My advice to women: never stop learning from each other and pass on the experiences you’ve been given. Take a look at what our mothers went through. They encouraged and uplifted our generation to shatter boundaries in the workplace. Now, we will assist our daughters (and sons) to continue to make the workplace and the world a better place for their children.
Unions and TPAs Serving America's Veterans - November 6, 2019

Benefit Programs Administration (BPA) stands with all of America’s veterans as they transition from military service to the private sector. Veterans returning to the workforce, like all workers, deserve fair pay and safe working conditions. They deserve access to the best benefits, job prospects and networking opportunities. After nearly 75 years of working with unions in the benefits industry, BPA has seen union membership offer many of these perks to help America’s veterans succeed after military service.
A significant protective program designed for veterans in the labor force is the Uniformed Services Employment and Reemployment Rights Act (USERRA), a federal statute that protects servicemembers' and veterans' civilian employment rights. This statute requires employers to put individuals back to work in their civilian jobs after military service. USERRA Advisor assists veterans in understanding employee eligibility and job entitlements, employer obligations, benefits and remedies under USERRA. However, USERRA is not the only assistance available to veterans after leaving the military.
Service members tend to be quick learners, hardworking, personally responsible and selfless, still, many of them have trouble attracting the attention of hiring managers. A recent article by The Hill expressed the overlooked need for veterans in the labor market. High-quality skills expected of military veterans include teamwork, leadership, structure, commitment, reliability, and punctuality. However, the years of firsthand experience that directly translate into IT, security, manufacturing, logistics, or managerial positions are typically overlooked by hiring managers. It is not a lack of knowledge, but a lack of communication between businesses and veterans causing this discourse. But with unions, veterans bring valuable benefits as a labor pool; for veterans, unions bring a rich network readily available to use and expand their knowledge and skills. Unions bring a network that connects veterans to the right people.
According to a study from the Institute for Veterans and Military Families at Syracuse University, veterans are more likely to seek out a position from an organization that offers competitive benefits and provides education on how military skills carry over into the workplace. Roughly 16 percent of veterans—or 1.2 million veterans—are in a union or covered by a union contract. Unions can help both veterans and nonveterans earn higher wages, obtain better benefits and assist with continuing education. On average, a worker covered by a union contract earns 13.2 percent more in wages and is much more likely to have health and retirement benefits than a peer with similar education, occupation, and experience in a nonunionized workplace in the same sector.
For veterans, union membership can be beneficial in more ways than just benefits. Union jobs often provide problems to be solved, possibly the chance to work with one’s hands, freedom from a desk, camaraderie and a sense of service. Depending on the job and experience, union members can earn over six figures a year, a healthy salary that eventually gives way to a robust pension.
After everything veterans have done for our country and our freedom, it’s only right that they gain access to fair wages, working conditions, and solid benefits, as well as a place they feel supported and enjoy working. Unions can help connect veterans to meaningful work with fair compensation, while also helping companies employ remarkable workers.
Veterans can rely on BPA for the administration of benefits plans through single or multi-employer trust funds. We work hard to earn your trust and work harder to keep it. Contact us to learn how you can partner with BPA to earn the effective benefits you deserve.
Judi Knore: "More Progress to be Made" - October 15, 2019

Women comprise 47 percent of the U.S. workforce and have fueled 51 percent of the workforce growth in the past ten years. At BPA, we stand behind gender equality in the workplace and seek to elevate women into leadership and supervisory roles. We believe that when we allow a diversity of opinions at the table, our organization flourishes. BPA’s Women in the Workforce is a monthly blog series featuring female employees from the BPA team discussing their personal challenges and triumphs in the workplace. Each woman offers her own insight into how to overcome these challenges, how impactful the support of women can be and how employers can help combat the problem of inequality at work.
Stop by exhibitor booth #908 at next week’s IFEBP Annual Employee Benefits Conference to chat with Judi Knore, as well as some of the other BPA women featured in our Women in the Workforce series!
Working for BPA, I feel like I’m a part of a family that is full of support and builds a nurturing environment. From the staff on the floor that interact with participants, to leadership, such as Hormazd, I’ve always felt at home here and I love working for BPA. I grew up in this industry – my father was a plan administrator and I saw what he did on a daily basis. I was hired 1993 as a pension processor and while working at different positions within the Company, have developed very strong relationships with both coworkers and the people I serve. Working as an administrator feels like something I was always meant to do; it’s in my blood!
As a woman in the workforce, I’ve never felt uncomfortable or out of place at BPA. I think because BPA is a family-owned business, we hold strong family values and management supports a balance of work and family responsibilities. As an example, I was promoted to Administrative Supervisor when I was seven months pregnant. Even in 2019, some women starting and growing their families struggle to continue to climb the ladder at work. However, my hard work has never gone unnoticed at BPA and I feel that I have been rewarded for my efforts.
Generally, women struggle to break through the “boys club” in the workplace. We feel like we need use sports-related ice breakers just to join the conversation. In some instances, women are seen as the domestic employees and are not given the same type of assignments as male employees. Fifteen years ago, while attending my first Board of Trustee meeting as an assistant administrator, a male attendee working in the industry asked me to get him some coffee during the meeting. At the time, it was much more uncommon to see women in meetings like that with an equal seat at the table.
On a positive note, recently we were reviewing investment reports with one of our clients when one of the male industry leaders noted that the key leaders in this particular fund were all men. He questioned why there seemed to be very few women on staff. It was enlightening to hear this perspective from a man who holds an industry power position voice this as a concern. We’ve come a long way in the last fifteen years, but there is still more work to be done when fighting for gender equality.
Employers can begin to address gender inequality in the workplace by being fully inclusive in promotions, day to day operations, and decision making. Everyone should get equal opportunities regardless of gender. BPA managed to prevent this issue by promoting from within the company. With the family aspect of BPA, everyone is recognized for hard work and people are recognized for that work – male or female.
The workplace in general is starting to open more doors and expand opportunities for women and we’ve come a long way since a decade ago, but there is still more to be done. Women have worked tirelessly in the past to be noticed and taken seriously in the workplace and some of those efforts have payed off. Women are deserving of equal opportunities in the workplace and employers should start advocating for us. I feel very fortunate to work at BPA where I am seen as an important and equal part of the company. I feel very at home here and I wish that feeling for other women in their place of work. With employees and employers working hand in hand for equality, I am certain we will get there.
Unions on the Front Lines Fighting Inequality - October 9, 2019

The 65th Annual IFEBP Employee Benefits Conference is just weeks away, and BPA is gearing up to head to San Diego. We’re excited to join industry peers to discuss important topics including gender equality, equal pay, the opioid crisis and mental health. While all of these topics span various industries, each of them has some root in combatting inequality. BPA has a longstanding relationship with labor unions who have been working to support their members in seeking equality in the workplace for decades.
Unions have been on the front lines of fighting inequality for decades. Due in large part to union involvement, the U.S. has created laws and regulations that prohibit child labor, allow for family and medical leave and enable employer-provided health care. Unions have been a catalyst for the ongoing civil rights movement, women’s rights, and closing the gap between rich and poor. Today, unions are continuing to fight for racial and gender equality, fair wages and treatment, and better working conditions. BPA is proud to work with union members every day. Especially in today’s political climate, BPA stands with their members to effect change politically and systemically.
Work mirrors many of the same issues that we face in society at large today. Therefore, unions have a unique position of being on the front lines to fight injustice and inequality, starting in the workplace and expanding beyond. In order to understand the value that union membership offers members now, it’s important to understand the history and impact of the organized labor movement.
Unions have been present in the U.S. since its founding. The earliest recorded strike occurred in 1768 when New York tailors protested wage reduction. The creation of the Federal Society of Journeymen Cordwainers (shoemakers) in 1794 is cited as the beginning of sustained trade union organization among American workers. Perhaps one of the most notable moments in union history was in 1866, when the National Labor Union was formed to convince Congress to limit the workday to eight hours. This marks one of the first successful union impacts on federal law. Since then, unions have continued to shape labor law and policy, such as:
The Fair Labor Standards Act - In 1870, the average American worked over 60 hours with no days off. Labor unions demanded shorter work weeks so that working-class people could spend time with their families instead of constantly working with no leisure time. The movement gained enough political momentum for the Fair Labor Standards Act to pass in 1937. The act limited the work week to 40 hours (eight-hour days), mandated workers be paid for overtime, and kept children under 16 from working during school hours.
The Family and Medical Leave Act - In 1993, labor unions brought forward the issue of time off work for matters such as a new baby, injury or illness, and other family obligations. Under the Family and Medical Leave Act, public employees as well as private sector workers who have worked for at least one year or 1,250 hours in the past 12 months are guaranteed 12 weeks of unpaid medical leave to care for themselves or their immediate family.
The Equal Pay Act - During World War II, more women began entering the workforce to replace the men who were fighting overseas. Despite working the same job, women were paid substantially less than the men they were replacing. The National War Labor Board endorsed equal pay for women for the duration of the war, but the initial Women’s Equal Pay Act failed to pass. The Women’s Bureau of the Department of Labor – along with an endorsement from Eleanor Roosevelt – helped the act to finally pass in 1963.
While workplace challenges have evolved, union members continue to be a driving force behind labor change. Just as unions continue to stand with workers, BPA continues to stand with its members to navigate the changing political climate and provide best-in-class counsel and support on benefits programs for members. Stay tuned to our blog and our newsletter for more updates on changes affecting our industry, and we will see everyone at IFEBP in October!
Dora Vele: "Support Goes A Long Way" - October 2, 2019

Women comprise 47 percent of the U.S. workforce and have fueled 51 percent of the workforce growth in the past ten years. At BPA, we stand behind gender equality in the workplace and seek to elevate women into leadership and supervisory roles. We believe that when we allow a diversity of opinions at the table, our organization flourishes. BPA’s Women in the Workforce is a monthly blog series featuring female employees from the BPA team discussing their personal challenges and triumphs in the workplace. Each woman offers her own insight into how to overcome these challenges, how impactful the support of women can be and how employers can help combat the problem of inequality at work.
I started working at BPA as a pension processor and have been with the company for 29 years. Throughout those years, I’ve learned a lot and have gotten support from leadership. BPA shows confidence in their people, and I’m proud to be a part of this company. In an environment like this, you can either sink or you can swim, and with the support the team receives from each other and our leadership, we are not going to sink.
Our CFO, Hormazd, has always been positive and supportive while helping female employees grow within BPA. In 2015, he presented me with the opportunity to be an administrator. I feel like I can continue to grow here with advice from great male and female mentors who are always happy to help. Everyone, from leadership to peers to trustees, were very supportive when I became an administrator. Many of them knew who I was and knew I previously worked behind the scenes at BPA. The support and appreciation for my hard work felt very rewarding.
I think the biggest challenge for women in the workplace today the boys’ club that still exists in some workplaces. These informal clubs where men wield power through their shared connections or backgrounds can understandably damage the confidence of working women. In some places, women have a harder time proving themselves and proving that they can do the same work as a man, but BPA doesn’t have this mentality-- we give both men and women equal opportunities to grow and succeed.
Professionals can help combat these types of issues. Unions are still evolving and pushing for new regulations in the industry. Some new companies are hiring more women in leadership roles, but there are still mostly men in those seats. Women are starting to make it to the top and hopefully over time, companies will start changing more rapidly for the better -- for women.
Benefit Trends Ahead: What HR Professionals Can Watch For In 2020 (HR.com) - September 30, 2019

The shifting policical landscape could bring large changes to the human resources and benefits administration industries. BPA Benefits' executive vice president Zane Dalal published an article in HR.com about how HR professionals can prepare amidst policy uncertainty.
An excerpt from the article can be found below.
The benefits landscape is ever-changing. It is a challenge for human resources professionals and benefits fund administrators alike to navigate the moving goal-posts of our industry as policies and requirements — such as individual mandates, new required minimum distributions and taxes on student loan benefits — change. From a legislative perspective, HR professional and administrators can expect changes that drastically affect the benefits industry over the next year, each bringing their own changes our industry should watch.
Supreme Court Rulings
In October, the Supreme Court will begin hearing cases for the 2019 term. This term, the justices will hear two pension-related cases.
What Employers can Expect from the New Generation of Workers: Trends in Gen Z Workers - September 10, 2019

Just when employers feel like they’ve learned how to cater to their millennial employees, a new challenge arises: what to expect from Generation Z.
The “Gen-Z” group, born in or after 1997, will outnumber Millennials in 2019. The oldest of the group are around 22 years old and are just entering the workforce. Almost half of Generation Z is non-white, making them the most diverse generation to date.
Just now entering the workforce, Generation Z will make up 40 percent of the working and consumer population by 2020. This generation already has a reputation for being hard workers and take responsibility for their career. Gen Z is more than willing to put in extra hours if they will be rewarded for doing so. They’re competitive and want to be judged by merit but prefer to work independently.
The newest generation to the workforce is deeply driven by security. Skill development and self-improvement are a big priority for these employees, as well as money and benefits. Up to 70 percent of Gen Z workers say salary is their top motivator, and that their top “must have” benefit is health insurance. Additionally, 35 percent of Gen Z plan to start saving for retirement in their 20s. These employees also expect work phones and laptops and expect texting and instant messaging to be essential to workplace communication.
Gen Z has an unprecedented digital connection – even more so than Millennials. They have never known life without technology at their fingertips, and use five screens on average: a smartphone, TV, laptop, desktop and iPod or iPad. A whopping 96 percent of the generation owns a smartphone, and more than half spend at least ten hours a day on an electronic device. However, Generation Z places high value on face to face interactions. These employees don’t just want to work for their employer – they want to be coached by their employer as well. Social experiences in the workplace also hold high value, which makes culture a key point for recruiting and retention.
Dubbed as the “We Generation”, Generation Z is the most advocate-friendly generation thus far. Born in the years right before and after 9/11, experiencing gun violence from a young age and coming of age in a time of political discourse, they are more likely to be politically active, and frequent businesses with socially responsible values. These employees expect no less from their employers.
Employers prepared to provide a positive day-to-day working experience with competitive conversation and quality personal and professional development will do well in welcoming Generation Z into the workforce. At BPA, we train our administrators to work with all generations of employees. We work daily to build lasting relationships with plan participants, and tout state of the art technology to keep employees and employers in the loop with their benefits year-round.
Annette Beatty: "Working Your Way Up" - September 4, 2019

Women comprise 47 percent of the U.S. workforce and have fueled 51 percent of the workforce growth in the past ten years. At BPA, we stand behind gender equality in the workplace and seek to elevate women into leadership and supervisory roles. We believe that when we allow a diversity of opinions at the table, our organization flourishes. BPA’s Women in the Workforce is a monthly blog series featuring female employees from the BPA team discussing their personal challenges and triumphs in the workplace. Each woman offers her own insight into how to overcome these challenges, how impactful the support of women can be and how employers can help combat the problem of inequality at work.
BPA is a great company where I’ve been employed for the last ten years. I’ve seen the potential this company has, including the many opportunities to grow, which I’ve already experienced myself. We’ve gotten better at adapting to changes in the industry and improvement in available technology.
So many women in the workplace are still lacking in confidence, struggling with the gender wage gap and equal pay, or not supporting other women. BPA is supportive of women in the workplace, employing and advancing women and providing greater opportunities. As a result, we at BPA are able to avoid many of these concerns. Unfortunately, that is not the case with all employers.
Employers can make a decision to level the playing field for women in the workplace. Actions such as women’s empowerment initiatives can provide opportunities for women to take on leadership roles and gain valuable management experience. Results of these programs include better company morale, more projects that require and encourage teamwork, continuous encouragement and support for women, more feedback and recognition, an increase in pay and better job titles, and more opportunities for growth.
Through my years of experience and building more relationships at BPA, I’ve become well-regarded in the benefits industry and have begun to build a name for myself, thanks to the opportunities awarded through BPA. My clients and colleagues trust me and enjoy working with me. I’ve also been able to branch out and take on new business roles and responsibilities that I wasn’t doing previously. The support of other women and my supervisors at BPA has allowed me to grow within the company, starting from data entry and working my way up to processing and then up to administration.
Because of this support, I’ve been able to attend board meetings and become exposed to the decision-making and accounting aspects of BPA. These changes have allowed me opportunities for development, more exposure to different courses, and the ability to network with employees who go to the annual employee benefits conference for the International Foundation of Employee Benefit Plans (IFEBP). In addition to the great relationships I’ve formed, I can continue to collaborate with the team, while also working with seasoned administrators.
BPA has been a strong advocate for female employees and is an industry leader in advancing women in the workplace. We see some of the same characteristics in of the unions we work, many already have a fair pay structure and emphasize finding the best employee for the job, regardless of gender.
However, I understand that a lot of women aren’t afforded the same support and unbiased pay structure. Employers looking for ways to support women in their businesses should become stewards that help represent employees if women don’t feel comfortable representing themselves, give general support to help women grow in the workplace, and ensure their female and male employees are being paid the same wage for identical work.
I have been fortunate to spend my career growing and learning at BPA. It’s afforded me opportunities I don’t think I would have had otherwise, and there’s a great support system here. I really encourage women to find their own support system among peers and leaders. My advice for women looking to advance in the workplace? Surround yourself with people who want to see you grow.
Can Benefits Reduce Employee Stress (HRCI) - August 15, 2019

The HR Certification Institute (HRCI) interviewed top benefits administrators, including BPA Benefits executive vice president Zane Dalal, in an article examining the correlation between company benefits and the stress levels of employees.
An excerpt of the article is below.
U.S. workers continue to report increasing stress levels, and anxiety-related issues affect an estimated 40 million adults annually. However, these disorders often go undiagnosed or untreated. This means you probably have employees who are suffering from stress and anxiety.
The good news is that you can help. Through comprehensive and unique benefits packages, you can reduce your employees' stress load.
Read the full article here.
Low Cost Benefits of Paid Time Off - August 14, 2019
Paid time off (PTO) is considered to be a monetary benefit that adds to an employee’s compensation package. More and more employers are implementing benefit packages that include a generous amount of paid time off, and by doing so, they’re recruiting better employees, retention rates are higher, and productivity in the workplace improves significantly.
By employing PTO, companies make quality employees feel happy, appreciated and motivated. When employees are happy, they tend to have increased performance and creativity. Their quality of work improves and they pay more attention to detail.
Although PTO is considered a benefit for the employee, there are just as many benefits for the employer. In most cases, the benefits of paid leave outweigh the expense. Payroll costs tend to be fixed, so that employers who offer paid leave will typically not see additional expenses from month-to-month. Increased morale also improves workplace safety, as employees tend to be less distracted and focus more on safety rules and the task at hand. PTO also decreases the amount of unscheduled absences from work, which gives employers greater predictability and the ability to plan work based on who will be in the office.
A research group called Project: Time Off created a study where employees rated paid vacation as the number 2 most-important benefit, after health care. Employees working in an environment that encourages vacations are more likely to use all of their vacation time (77 percent compared with 51 percent). However, the study found that employees who reported encouragement to take vacation from their employers (68 percent) are much happier with their jobs than those who work at places where either vacation is discouraged or managers are ambivalent about taking time off (42 percent).
Companies are starting to target younger generations entering the workforce when it comes to new hires. Millennials are prioritizing generous benefits over other services and perks. Project: Time Off’s study found that millennials use a greater proportion of their days for travel than Generation X or Boomers. Implementing generous PTO policies will be more appealing to young job seekers and create competition among companies who don’t offer PTO, or companies who offer a standard 10 paid vacation days per year.
Not all employees enjoy taking a luxurious vacation somewhere warm and tropical for two weeks out of the year. Some choose to take a staycation, or a “mental health day” to simply stay at home and recharge after a difficult work week. After doing so, they return to work more energized and motivated. If employees must wait an entire year to get a week of vacation, they’re more likely to feel burned out, their productivity decreases, and they may lose interest or passion for their job.
Taking time off work for mental health care is still a stigmatized practice, which might explain why half of employees use their PTO for mental health days, but say they don’t report them as such to their boss. Nearly a quarter (24 percent) of U.S. employees surveyed say their biggest vacation using PTO last year was a staycation at home. Mentally healthy employees have a healthy work-life balance. If employees don’t feel like they’re getting enough time off to recharge, they’re going to feel those effects both inside and outside of the office. PTO is a flexible option for rewarding employees and boosting morale in the workplace.
By giving employees generous or unlimited vacation days which include sick days, companies are avoiding an endless cycle of illness among employees. Research shows that 69 percent of workers don’t take sick days even when they are really sick, which puts coworkers at risk. Workplace illnesses cost employers $160 billion every year in lost productivity. It’s important for employees to feel like they can use their time off when they’re actually sick to avoid an illness spreading cycle.
At Benefit Programs Administration, we deliver outstanding services with personnel who are passionate about a healthy work environment and putting people first. BPA is proud to work with companies and union representatives to manage benefit plans for union workers. Whether you are just starting a group plan for your employees, self-administering a plan, or currently employ administration that may not have the proper skills, BPA can help you find the best solution for your plan and its members.
Selene Calderon: "You Have to Believe in Yourself" - August 8, 2019

Women comprise 47 percent of the U.S. workforce and have fueled 51 percent of the workforce growth in the past ten years. At BPA, we stand behind gender equality in the workplace and seek to elevate women into leadership and supervisory roles. We believe that when we allow a diversity of opinions at the table, our organization flourishes. BPA’s Women in the Workforce is a monthly blog series featuring female employees from the BPA team discussing their personal challenges and triumphs in the workplace. Each woman offers her own insight into how to overcome these challenges, how impactful the support of women can be and how employers can help combat the problem of inequality at work.
I started working with BPA right out of high school, came up in this industry and was mentored in the workplace. When I started with BPA, there was one female partner who tried to join the other male partners for lunch at a nearby club, but they wouldn’t let her in because she was a woman - even in 1986 California! It’s been a systemic issue; sometimes, older male generations will look right past you to the man sitting next to you, even though you’re the one doing the work.
Today, I feel a great deal of pride and fulfillment to be able to see the positive strides made since the beginning of the company. Thanks to Zane, Hormazd, and the mentorship of my peers, I’ve been able to grow into a Vice President role at BPA. These people make me feel respected, realizing that I’m trusted and appreciated each day. Everyone has a voice and everyone’s opinions are not only heard but sought after. However, I also realize not every woman feels this way at work.
I think one of the biggest challenges women currently face in the workplace is not seeing their own potential or abilities. Women do not feel empowered in the workplace and do not receive the mentorship or tools they need to pursue their goals, dreams and new endeavors. Although there is always room for growth and improvement, there is more potential than one would recognize. This struggle dates back as far as 1978 when Pauline Rose Clance and Suzanne Imes studied the “impostor phenomenon” in high achieving women. They found that societal gender stereotyping appeared to contribute significantly to the development of the impostor phenomenon. Women are far more likely to feel like their accomplishments are attributed to luck, instead of their own ability.
Women are still struggling today to feel empowered in the workplace and embracing their confidence. A major enabler of this problem in my opinion is social media. These new media platforms give off a false reality that everyone else is doing better, being better, looking better -- but in reality, not everything, including the bad, is being shared. As the senior women in the office, we have a responsibility to help the young women just starting their careers understand that they add value to the company and to the industry. If they’re willing to break out of their shell, they can progress and grow into higher positions. I want to return the mentorship I’ve received to future generations of women, giving them the tools and resources to continue growing in this industry and in their lives.
Thankfully, there is an increase in unions advocating for women’s issues, just as there is an increase in women’s membership overall. The Office and Professional Employees International Union (OPEIU) trust funds – which are predominantly female – represent women in the workforce. No matter what the position, they’re advocating for women to have working wages and benefits that support their families. Today, there are even women in traditional male trades. Unions have opened their arms to females and continue breaking down barriers.
Working in the benefits administration industry, I’ve witnessed an industry that was once dominated by male administrative positions, transform into an industry with more female administrative opportunities. Today, women are making big decisions and contributing to the growth of the organization. From my own experiences and personal growth, I’d like to tell all females -- don’t be afraid to go to a board meeting because there are all men in the room. My advice for women looking to advance? You know what you know, and you have to believe in yourself.
An Update on the Opioid Crisis - July 23, 2019
Every day, more than 130 people in the United States die from an opioid overdose. It’s the deadliest drug epidemic in the modern era. Fortunately, unions are continuing to step up in force to fight for their members. Unions fight for the wellbeing of workers on the job, however, that commitment must not only focus on the physical aspect, but also the mental aspect of workers. Employee mental health can be even more long-term than any physical injury and that includes an addiction to opioids.
Construction is a significant work environment prone to injury and addiction and the overdose rate is seven times greater than for the general population. According to Jill Manzo of the Midwest Economic Policy Institute, the opioid epidemic in the Midwest construction industry cost an estimated $5.2 billion in 2015. Each construction worker with an untreated substance abuse disorder costs an employer $6,800 per year in excess healthcare expenses, absenteeism, and turnover costs. But when a construction employee is in recovery from a substance abuse disorder, lives are saved and contractors save nearly $2,400 per year. The construction industry has some of the oldest multi-employer plans in the country and BPA has served construction workers from the very beginning.
Additionally, auto plants continue to be prime working environments for addiction. Repetitive and physically demanding labor often leads to injuries followed by chronic pain. Generous medical plans with low-cost drug pricing, on top of the lack of knowledge many doctors have regarding the serious addictive qualities of these drugs, creates problems for many union members, not just auto workers.
However, the UAW is making the treatment and prevention of opioid misuse a top priority on their list of issues during this year’s contract negotiations with the Detroit 3. Many feel that the issue demands that unions get involved and combat this issue in a positive way. A strong partnership between the unions and the companies are just one step in the right direction to saving lives.
Unions are continuing to combat this crisis through assistance programs, peer advocacy training, courses about substance abuse, and training on proper use of Narcan. The National Institute on Drug Abuse (NIDA) reports that more unions are utilizing employee assistance programs (EAP) that offer counseling and short-term assistance for people needing help with drug and/or alcohol abuse. EAP services have helped workers transitioning back to work after an absence for addiction treatment programs or services.
Union programs are gaining traction, and more research is being done to end the opioid crisis. The National Institute of Health (NIH) is joining private partners to launch an initiative in three scientific areas: developing better overdose-reversal and prevention interventions; finding new, innovative medications and technologies to treat opioid addiction; and finding safe, effective, nonaddictive interventions to manage chronic pain.
Additionally, some important labor relations guidelines to be aware of include disability being a protected class and can apply to members who are addicted to opioids, employee benefit programs that help members affected by the opioid crisis, and opioid abuse resulting from treatment of a workplace accident can be a covered “consequential condition” and, if so, treatment is free to the member.
Though the crisis is far from over, important measures have been taken and the situation is slowly, but surely, improving.
The Importance of Employee Mental Health - July 16, 2019

It’s no secret that a productive work environment stems from happy employees. For most Americans, a large part of their daily lives is spent at work. According to Mental Health America, less than one third of Americans are happy with their work. Not only does this decrease productivity from employees, but it also puts employees’ long term mental health at risk. In order to improve productivity in your business, there must be an awareness and understanding of the workplace environment and how it can be adapted to promote better mental health for your employees.
There are many different reasons why employees are unhappy with their work environment. Some of those reasons include minimal wage growth, lack of opportunity to advance, lack of teamwork and unhealthy co-worker relationships, excessive labor or hours, and poor management and communication practices. These factors add a strain to employees’ wellbeing and the day to day lives outside of work, too.
Smaller businesses may feel the financial hit even harder when impacted by poor employee mental health because there are fewer resources and employees to prevent or manage these problems. An increase in mental health problems for employees can affect businesses by an increase in absenteeism, conflict, turnover, loss of productivity, increase in cost, greater risk of accidents, injury, or incidents, and burnout.
Fortunately, there are ways your business can promote a healthy work environment for its employees and reduce the risk of negative mental health. First and foremost, understand the opportunities and needs of individual employees and develop better policies and emotional support. World Health Organization recognizes that interventions in the workplace can also protect and promote mental health, which include implementing and enforcing health and safety policies, involving employees in decision-making, encouraging a work-life balance, creating programs for career development and growth, and recognizing and rewarding the contribution of employees.
At Benefit Programs Administration, we deliver outstanding services with personnel who are passionate about a healthy work environment and putting people first. We have a proven record showing trustees can count on us. We’ve built long lasting and trusted relationships with our employees, trustees, and partners, and with the support of our responsive customer care team we offload complex, time-intensive plans so our trustees can manage healthy time management.
A happy workplace makes for happy employees! Trust is one key factor that builds strong relationships in the workplace and strong relationships make for a great TPA. Contact us to learn how you can partner with Benefit Programs Administration to build the trust that propels and motivates workforce and healthy employee mental state.
Working For You: A Day in the Life of Your Benefits Administrator - July 9, 2019

Benefits administrators provide human resource services and advice for both employers and employees within a unionized organization. They manage the directing and planning of all day-to-day operations of a group benefits program for unionized workers. This includes group health, dental, vision, worker’s compensation, short-term and long-term disability, travel and accident plans, life insurance, flexible spending accounts, health savings accounts, 401(k) plans and other retirement options.
The Taft-Hartley Act reserved the rights of labor unions to organize and bargain collectively. Under the Taft-Hartley model of a union/multi-employer-based benefit plan, a benefits administrator must know and follow company policies, state regulations, and federal laws. They must stay up-to-date with any policy or regulatory changes, respond to problems, prepare reports, and develop relationships with employees and vendors to do their job well.
BPA is proud to work with companies and union representatives to manage plans for union workers. Our committed staff is focused on providing best-in-class service to workers and offering valuable insight on developing regulations to employers.
Lance Phillips is a Vice President and Administrator at BPA, and has worked with BPA for 30 years. An invaluable member of our team and trusted administrator to his clients, Lance exemplifies the high-quality customer service that BPA provides.
We sat down with Lance to understand how he feels he best serves plan members, regulation changes and more about his typical day at BPA.
What does a typical day-to-day look like? Or is it quite varied?
It varies. Depends on the time of year, the month, the quarter. On an annual basis in the fall, all of the health and welfare plans offer open enrollment to the participants. So, in September you’re working on open enrollment meetings and compiling information materials for participants. In October you’re sending those things our and requesting a response, then of course you receive the response and need to act accordingly. You work on behalf of the employees, as a liaison with new providers and a board of trustees, adjusting benefit categories - new vision/dental, etc. - and more. But it tends to come in cycles. Open enrollment is just one example.
How has the job changed since you first started?
Technology. There’s been an evolution from doing most work through the telephone to working through email. Providing data through email. Previously data came through a package, then fax, and now it’s all on the Cloud. Everything’s more immediate, but I think it’s for the better. It allows us to act quickly to better serve our participants.
How do regulation changes affect how you work?
The Affordable Care Act had a huge impact on all of the health plans administered. Regulatory changes are always ongoing with retirement plans. How is the PBGC going to survive when you have a lot of these plans that are under-funded? The BPA team reads the information that’s provided in the mainstream media and works with professionals – legal professionals, actuaries, consultants – to get into the nuts and bolts and what affect the legislation has on plans. How do we comply? How do we communicate the changes? BPA plan administrators are constantly learning and reacting to the changes that occur so that we can provide the best information and choose the best actions. It’s a team effort. We rely upon trust counsel to decipher the changes to the plans that we administer.
What would you say is the most important part of your job and why?
Being responsive. We aim to be as responsive as possible to other professionals by keeping them in the loop, answering their requests, managing participant requests and providing information, and being responsive to the companies we serve. When I think of administrators, we’re the quarterback. We need to make sure that everyone we’re working with on the team has the same mindset towards what needs to get done. Board of trustees, the company at large, and the staff internally.
The BPA benefits administrators are well-educated leaders in their field. BPA’s proven record is one that trustees, plan professionals, and participants have come to rely on. Whether you are just starting a group plan for your employees, self-administering a plan, or currently employ administration that may not have the proper skills, BPA can help you find the best solution for your plan and its members.
How to Attract and Retain Millennial Workers - July 2, 2019

The age definition of a “millennial” can vary depending on who you ask, but generally, millennials are defined as those born between 1981 and 1997. According to U.S. Census data interpreted by Pew Research millennials are set to soon overtake Baby Boomers as America’s largest generation.
As Baby Boomers and Millennials both age, America is seeing a greater influx of Millennial immigrants, giving the group an edge in outgrowing Baby Boomers.
Why does this matter?
Soon, millennials are going to be the largest generation in the workforce. They currently have the reputation of being disloyal “job hoppers” but they have been entering the workforce at challenging times, enduring three recessions in the last 20 years – 1998, 2001-2002, and the Global Financial Crisis in 2008.
Regularly, millennials chose to make compromises when entering the workforce, especially during the Global Financial Crisis. They saw their elders, who had for years been loyal to their jobs, laid off. Their peers were turned down for jobs that their education promised they would find. Most millennials at this point in their lives have had four jobs and will move around to advance their career.
Fostering Millennial Loyalty
In contrast to these misconceptions about millennials, they are actually extremely loyal workers. However, business owners must work harder to earn millennial loyalty and trust. As this group of workers age, they are prioritizing good benefits, saving for retirement, homebuying and debt payoff. They care more about benefits than employers have given them credit. Using tactics that appeal to millennials to market benefits packages and the services that accompany them will be a make or break for employers aiming to attract and retain millennial workers.
Use new enrollment and benefits technology to appeal to millennials. Millennials grew up with quickly evolving technology. Therefore, it’s important to them to have easy access to information and services. Leverage well-designed online platforms, mobile applications and service providers with good online user experiences.
However, keep it simple. While millennials love using technology to make their lives easier, they also expect a simple process to reach human, non-automated customer service associates. In a day and age where technology plugs people into a bombardment of information, no one wants to be bogged down by extraneous and complicated information or steps.
Allow for flexibility and customization in benefits packages. Millennials know that these days, one size does not fit all. A benefits package that can be customized can go a long way.
This doesn’t mean a new and unique package for each employee. For example, an employer can offer a base health insurance plan, with the option for extra coverage - such as increased dental, additional PTO, tuition support or professional development stipends. Providing employees with new customization options at certain life milestones can also be a good way to secure long term commitment and loyalty from millennial workers. For example, remote and telework options after having or adopting a baby.
Highlight preventative coverage elements. For all their immediate concerns – finding a job, student loans, navigating adulthood - their health isn’t something many young workers consider.
However, millennials are emphasizing embedding good health habits and taking care of their wellbeing at an earlier stage in life. Robust preventative care elements – such as free flu shots, gym memberships or stipends, nutritional advice and workplace wellness events – can go a long way in expressing that you care about your employees.
At BPA, we’ve seen the numbers. Millennial membership in unions is rising right along with their rise in the entire U.S. workforce, and we’ve evolved with them. Our state-of-the-art technology provides the best customer service for plan participants who wish to work online, but there’s always someone at the other end of the phone, should personal assistance be necessary. We work with you to develop and maintain the trust of plan participants of all generations. We are committed to providing service that puts people first.
BPA Statement on Supreme Court Department of Commerce v. New York Decision - June 27, 2019
We are supportive of today’s Supreme Court decision in Department of Commerce v. New York to refrain from including a citizenship question as part of the 2020 Enumeration Census. However, we remain concerned that this case has been sent back to the district court for further explanation and review by the Department of Commerce. By its very name, the census is designed to count “the whole number of persons” regardless of legal standing or citizenship, within any given jurisdiction, in order to ensure accurate dispersion of federal funds. Today’s decision offers a potential gateway for the Administration to continue its efforts to overlook organized labor and union members and marginalize minority voters. The decision also makes no mention of the eleventh-hour additional evidence affecting minority voters and the attempts reshape electoral maps to favor one political party over another.
We at BPA stand alongside our members, committed to compassion and support for all individuals. Our fund participants are and will continue to be our foremost priority. We are steadfast in our efforts to ensure that all persons feel safe and supported in the communities in which they live and work and retain the right to fair voting practices and electoral maps. We will continue to provide best-in-class management to our participants, as well as serve to advance and protect their interests on a national political scale.
In today’s legal opinion the Court affirmed that the Citizenship question was not only constitutional but that the Census Act devolves the complete power of Congress in regard to the Census to the personal discretion of the Commerce Secretary. The opinion of the court authored by Chief Justice Roberts upheld the right of the Commerce Secretary to act at his discretion and supported the idea that he could do so with political motives consistent with the Trump Administration. This statement means that while it is possible we will not see a citizenship question on the 2020 Enumeration Census, this decision solidly paves the way for the question to be included in the future.
This incremental tactic is vintage Chief Justice Roberts, reminiscent of the ruling in National Federation of Independent Business v. Sebelius, which allowed the Affordable Care Act to more forward, yet also be reversed in part. While technical reasons for remanding the decision to a lower court take into account the false and disingenuous rationale given by the Commerce Secretary for this agency action, the remand seems to be in keeping with the intent of the Chief to rebrand his court as an impartial arbiter of justice, but also avoiding political backlash in a Presidential election cycle.
Enrollment Technologies Up Employee Plan Participation - June 25, 2019

Technology powered enrollment platforms are replacing manual methods to make it more efficient for businesses to enroll employees in retirement, health and welfare benefits plans. Along with other advantages, we have seen a drastic uptick in employee enrollment technologies used to facilitate employee participation in benefit plans.
For instance, many plan sponsors are electing to shift from manual enrollment to auto-enrollment, meaning employees are automatically re-enrolled into coverage without needing to fill out any additional paperwork. However, auto-enrollment does come with an opt-out provision.
Surveys show that employees increasingly trust employers to offer appropriate plan options for them, thus they are more open to auto-enrollment than ever before. In fact, according to a study conducted by the Consumer Federation of America on long term disability insurance, 85 percent of disability beneficiaries agreed that employers should auto-enroll all new employees in disability insurance. Employees understand that auto enrollment helps them avoid inadvertent disruption of vital benefits like disability insurance. Additionally, an employee who had selected a plan that covered the specific medical needs of a dependent child or spouse would not have a lapse in critical coverage with auto enrollment. As for retirement, auto enrolling employees in certain investment plans makes their portfolio grow. This is particularly useful for those who have not been able or did not select an investment option where a choice was available.
Several plan sponsors have opted for this already.
Younger employees would do extremely well if auto-enrolled into a 401k match. At the current rates, an employee who starts a 401k in their 30s is likely to have approximately $600,000 upon retirement. Whereas an employee joining a 401k in their 20s, who harnessed the compounding power of an extra decade, stands to gain closer to $1M.
These interrelated trends reverse the longstanding and purportedly less efficient alternative of manual employee elections, such as the selection of health care plans during open enrollment. Additionally, auto-enrollment may encourage plan participants to invest early and more often. Web-based technologies facilitate employees' retirement planning by delivering integrated investment plan information – specific to the employee – along with automated re-enrollment reminders.
Technology not only eases the enrollment process for employees by ensuring they have all needed information at their fingertips, but it also benefits employers. Transitioning from pen and paper to electronic processes reduces the administrative burden on employers, while increasing accuracy and transparency during the enrollment process.
Auto-Enrollment Benefits At A Glance
- • Expedites the enrollment process through use of technology, offloading the traditional administrative burdens
- • 24x7 connectivity enables fluid communication between employees and human resource departments, through tools such as autoresponders
- • Empowers data tracking and mining of information so employers can identify meaningful employee patterns
- • Improves quality of support through employer-specific services, maintenance and reporting
- • Increases processing accuracy via standardized rule-based processes and forms
- • Allows for secure online data imports and exports, providing a richer user experience
As auto-enrollment continues to pick up speed, we are seeing the debut of more and more technologies focused on automation and employee engagement. Some systems even offer a tailored approach based on the needs of individual firms and their employees – including setting up carrier relationships with enrollment data, designing plan selections and integrating this data with enrollment platforms. Some systems even go a step further in offering ancillary web-based services connecting carriers to the platform, making for an even more robust employee experience.
For instance, some carriers offer their rates, underwriting guidelines and benefits options online, reducing the need for employees to turn elsewhere to seek answers to questions about plans offered.
Additionally, these tech-centric platforms can provide training and technical support on a range of topics, such as eligibility rules that can be complex and subject to change. Online communications can be personalized to employees, enabling employers to interact with their workforce in ways that promote loyalty, serving as tangible evidence that a business is invested in the wellbeing of its employees beyond the workday.
An auto-enrollment system enables firms and their employees to derive all of these benefits without disrupting day-to-day operations. Added benefits offered on many of these systems include: system trainings; standardized enrollment forms and communications templates, such as email autoresponders; and best practices, tips and tools geared toward promoting user satisfaction.
Enrolling in benefits plans can be stressful for employees – especially knowing that health care deductibles may soon be on the rise. Many employers are shifting from full-coverage to high-deductible plans, with employees absorbing more out-of-pocket expenses than ever before. The multitude of plan options and continuous changes combined with the transfer of more costs to employees can be overwhelming.
Implementing automated-enrollment solutions demonstrates to the workforce that employers are actively working to remove some of that stress by prioritizing employees’ needs. Plan sponsors who adopt technology powered benefits platforms not only can facilitate and ease the plan selection process for employees, but they also have the ability to empower employee engagement at unprecedented rates.
BPA is equipped with the technologies to maximize benefits for employees and make reportable, trackable more efficient data for plan sponsors to maximize their financial strategies.
Benefit Trends in 2019 - June 18, 2019

Benefits are an important part of an employee compensation package and in many cases can be a determining factor for an employee in a job decision. Businesses need competitive benefits such as healthcare and retirement options in order to attract and keep employees. While there are many benefits that are traditionally offered, such as a 401(k) match or paid sick leave, the benefits that are the most valuable to employees change every year, influenced by new generations entering and growing with the workforce, among other factors. In 2019, workers are looking for companies that trend toward benefits in health, financial, and personal categories. Here are a few trends this year:
A Focus on Health Benefits
- Account-Based Health Plans - Employer healthcare plans often come with a high-deductible. Supplementing that plan with a health reimbursement arrangement (HRA), health savings account (HSA) or a flexible spending account (FSA) enables employees to cover extra or preferred expenses that may not otherwise be covered.
- Direct Contracting - The rising cost of healthcare and medicines are pressuring employers and their workers to contract directly with doctors and hospitals. This often improves access to better-quality care while lowering the cost.
- Emotional Health - Society is becoming more open about discussions on emotional, mental, and behavioral health. Companies are now offering benefits to address those challenges through counseling, therapy, and employee assistance programs.
- Wellness Programs - Employer wellness programs that incentivize healthy living is a common perk. In some cases, companies offer fitness center passes as well.
An Increase in Desire for Financial Benefits
- Retirement - Employees look to their employers for financial security. Setting up a 401(k) and offering employer matching is incredibly lucrative for many employees.
- Tuition Reimbursement - For companies and individuals to stay competitive, they need to be up-to-date on the latest industry knowledge. Tuition reimbursement for some means paying off their student debt, while for others it means being able to take classes and continue their education.
- Bonuses - Bonuses are typically merit-based. Incentive bonuses can increase employee morale and reward employees throughout the year.
A Trend Toward Innovative Personal Benefits
- Remote Work - Remote work has grown by 140 percent since 2005 and increases each year. Flexibility matters a lot to employees and offering remote work as a benefit is one of the best ways to promote a work-life balance.
- Family First - Companies are beginning to implement or enhance parental-leave benefits, offering an equal share of paid leave to both mothers and fathers. Additionally, some companies are offering on-site childcare.
- Unique Benefits - Whether it’s an arcade room in the office or beer stocked in the fridge, companies are beginning to offer benefits that reflect their overall culture. Knowing your employees and what they value goes a long way.
Benefits packages are continuously evolving; however, healthcare and retirement options will always be of value to employees. Employees are depending more on their employers for advice and education on how to leverage their benefits and how to maximize their usage. Third-party Benefit Administrators, like BPA, can help you navigate your employee benefit plan, offering insight into the latest trends and policy developments that impact your members.
Understanding Your Healthcare Payment Options - June 11, 2019

The cost of prescription drugs has become a prevalent topic in the United States. According to one study by Health Affairs, the prices of brand-name oral drugs increased by nearly 10 percent since 2008 and the annual cost of injectable drugs rose by more than 15 percent.
America patients are learning how to cope with these rising costs, often going into debt to pay for medicine or choosing to go without. Prescribed medicines are often preventative of larger health issues that could develop if ailments are left untreated. Employers who ensure that employees are able to get the drugs they need to stay healthy save their company money and resources.
Employers can help employees stay healthy while keeping costs low through educating employees on their options. A Flexible Spending Account (FSA) or Health Savings Account (HSA) are supplemental to company healthcare plans, helping both companies and individuals alike keep their healthcare costs down.
Flexible Spending Account
A flexible spending account (FSA) is an account to put savings for certain out-of-pocket health care costs. These accounts can be used to pay for copayments, deductibles, specified drugs, and other items as specified in the plan. The money contributed, either by employees or employers, to FSAs are not taxed, which means extra savings for all contributing parties. Both employees and employers can make contributions, making it a viable option for extra healthcare expenses not covered in the company plan.
FSAs have a plan limit of $2,650 per year per employer. The recipient of the funds must use the money within the plan year, but an employer can offer a “grace period” of up to two and a half extra months to use the funds. Another option is to allow a carry-over amount of up to $500 to use the following year.
To use an FSA, employees will need to submit a claim through their employer with proof of medical expenses and a statement showing that their healthcare plan doesn’t cover the cost. Employees will be reimbursed accordingly.
Health Savings Account
Most health insurance providers offer Health Savings Accounts (HSAs), which enable companies and individuals to pay for deductibles, copayments, coinsurance, and other medical expenses. Individuals can qualify if they are enrolled in a high-deductible insurance plan. Contributions to HSAs are not taxed before funds are placed in an account or after funds is withdrawn. Employers can also make contributions, which are not subject to federal income tax.
HSAs have a contribution limit of $3,400 for an individual and $6,750 for a family. Adults over 55 can add an additional $1,000 if they choose. If the HSA is set up through the workplace, employees can set up automatic contributions from their paycheck. Unlike an FSA, the account balance rolls over year to year, so an employee doesn’t have to worry about losing their savings.
Once an HSA is set up, the employee will receive a debit card or checkbook linked to their balance. They’ll be able to pay for their medical expenses directly instead of waiting for reimbursement.
How Employers Can Help
Talk to your employees about their healthcare payment options. Employees who are informed make better decisions about their healthcare spending, often saving companies money in the long run.
The time and labor involved in managing various healthcare options can be overwhelming and unmanageable for businesses. Additionally, as health policy continues to be a top item of debate, changes may occur that affect your employees. Staying abreast of these policy developments is important to ensuring effective benefits administration. Partner with a trusted Third-Party Administrator like BPA to make sure you’re utilizing the full benefit, as well as saving time, energy, and money.
Why You Should Partner with BPA for Your Benefits Administration - June 4, 2019

The Administration of Benefit Plans is a complex process and one that has become even more nuanced in the last decade. Whether a plan is governed under the provisions of ERISA or not, it is likely that in today’s working environment, the benefit offered is less an additional perk than it is a vital lifeline to the lives and families of many working Americans.
Quite rightly, the prudence with which these plans must be administered, has resulted in an ever-strengthening legal framework and its corollary policing measures, to ensure that contributions made to a plan fund, result in the intended and expected disbursement for the beneficiaries.
The Taft-Hartley model of a union/multi-employer-based benefit plan, is a familiar notion to most of us in the industry. However, in the age of mega-corporations and a Generation Z workforce, new plan models that seek to provide new benefits to suit new societal needs makes managing benefits more and more complicated. Managing these plans, now more than ever requires a deeper knowledge of benefits, the legislative and policy changes that affect them and the importance of prudent operations in the interests of the plan members. Whether considering the older Taft-Hartley Defined Benefit (DB) plans, the Defined Contribution (DC) plans and the variations on the 401k or the more recent Retiree Medical Trusts, HSA’s or uniquely operated ‘carve out’ plans- it’s one of many reasons why more and more companies are partnering with Third Party Administrators like Benefit Programs Administration (BPA). In the business since 1952, long before much of the federal legislation was written, with a proven track record of negotiating a changing environment, BPA is at the forefront of a new era of plan administration.
The BPA team are well-educated leaders in our field, with a proven record that trustees, plan professionals and participants have come to rely upon.
We are committed to relationships. We know and value the need for all those involved in plan administration to work together as a team, and we foster that team environment.
We provide better operations and better service. BPA’s technology in conjunction with its experienced longevity provide for a unique combination resulting in better operations for plan sponsors and better service for their members. Understanding the complexities of plan management and tailoring modern technologies to drive them, sets us apart from the ‘cookie cutter’ approach of competitors.
We understand the rapidly changing legislative landscape. Our experienced benefit administrators are well-educated and informed regarding the multiple Federal and State regulations governing the operation of even the smallest plans. The legal obligations governing every single employee benefit plan, whether small or large, healthcare or retirement, training or supplemental, are frequently too onerous for plan sponsors or employers to manage on their own. BPA provides trusted ‘third party administration’ that removes the everyday burdens of plan management, while operating in real partnership with plan sponsors, allowing our clients to focus their time on building their business with the understanding that their benefit plans are being executed and managed effectively.
We know the industry. BPA has long-standing relationships with industry professionals – relationships that we leverage to better support our clients. No matter whom your current professionals may be, from investment managers and actuaries to consultants, healthcare carriers and insurers, the chances are BPA can seamlessly partner with them or has already built a sturdy relationship.
We offer a best-in-class customer solution. BPA is a responsive TPA, where no task is too small for attention or too big in scope. BPA’s team-based approach to plan administration means that there is depth and breadth at every level of operation. Plan sponsors know that their data is well used, their benefits well disbursed and their members well looked after.
Whether you’re just starting a benefit plan, self-administering a benefit plan but feel snowed under with the task, or currently employ administration that may not have the experience, the skills and the tools, Benefit Programs Administration can help you to the best solution for your plan and its members.
Staying on Target for Retirement - May 28, 2019

Retirement, whether far off or right around the corner, is something everyone should be thinking of as they plan for their future. As with most things, proper retirement planning needs quality control measures for a smooth process overall. Knowing how to stay on target with your financial goals can be overwhelming, so here are some recommendations.
Start Early
The earlier you begin saving for your retirement, the better. Early in your career, it can be difficult to prioritize retirement savings, especially with student debt, rent, and other living costs that are competing for your attention. However, financial obligations never go away, and retirement savings are something that should always be included in the budget plan. Start putting aside a percentage of your paycheck and increase it by 1 percentage each year. If you put aside 6 percent at 25 years old, you can reach the recommended 15 percent by the time you’re 35 years old. This number includes employer contributions. The difference between saving a small amount, say $100 dollars a month, starting when you're 25 years old as opposed to 35 years old, can mean the accumulation of almost double the total amount by the time you turn 65. The power of compounding rests entirely with the timeline.
Take Advantage of Employer Programs
If your employer offers a company 401(k), see if there are associated benefits. Max out the percentage contribution for employer matching and if there is an option for automatic increases, sign up. These simple steps put savings on auto-pilot. If you’re ever too busy to monitor your account, at least you know you’re putting aside savings automatically.
Look at Investment Options
Most 401(k) accounts offer investment options that balance risk and reward, depending on preference. Management fees and fund expenses of remained level or, in many cases, declined. This has made the 401(k) option more accessible for the average American.
Know Your End Goal
If you plan to retire at 65, you can work backwards to calculate savings benchmarks. Creating savings goals based on your end date is a good way to ensure you stay on target for your retirement year. Make sure you set realistic goals. Setting savings too high might be discouraging and setting it too low can lead to a false sense of security.
Catch Up Contributions
If you’re behind on your goals and approaching your 50s, consider catch up contributions. Catch up contributions allow you to make additional contributions to your 401(k) or IRA. Even though this is a great way to expand retirement savings, very few people take advantage of it. Depending on the plan, you can contribute up to $19,000 in extra savings.
Be Aware of Social Security
The age to reap retirement benefits from Social Security was recently raised from 62 to 67. Traditionally, blue collar workers have retired earlier than white collar workers so if you’re planning on retiring earlier, you’ll need to make sure you have the savings to support it. Additionally, those who earn more money will receive a smaller portion of their income in retirement from Social Security. You’ll need more assets to round out your savings. If you’re looking to retire around age 65, you should aim for assets totaling between eight and 14 times your preretirement gross income.
It’s never too early to begin planning for retirement, and it’s never too late to start saving. Talk to an expert today to make sure you have the tools you need to stay on track.
The Top Seven Trends in Employee Engagement - May 21, 2019

Employee engagement is one of the most important differentiators among organizations this year. Employees have strong emotional ties to their roles and organizations; studies show that employees who feel like part of a larger mission, are aware of the ways their work helps them grow, understand the impact they have on others and are more engaged in the workplace.
Higher employee engagement also results in higher customer satisfaction, improved productivity and greater profits. How can employers ensure that their employees are feeling engaged?
Purpose at work. Engaged and successful teams are made up of people who feel a sense of purpose - 57 percent of younger Americans feel that the most important factor of employment is personally enjoyable and meaningful work. Studies also show that feeling a sense of purpose in life is linked to longer lifespan, better resilience, better health and improved sleep.
Employee experience. Employee “experience” – the observations, thoughts, feelings and engagements of an employees’ time at an organization – has risen to the top as one of the biggest employee engagement trends for 2019. Experiential organizations, who rate highest in culture, technology and physical workspace, outperformed their peers by 400 percent in profit, saw 40 percent less turnover and had stock prices that outperformed the general market.
Employee wellness. Companies with strong physical and mental wellness programs have employees who perform better and feel more engaged with their work. Creating a successful wellness program requires team buy-in but creates great return. These programs foster workplace camaraderie and provide teams a common goal outside of work.
Flexible work schedules. In a recent survey, 76 percent of respondents said a flexible work schedule is the best incentive their employer can offer. This trend allows workers to stay engaged on their own terms and work on their natural productivity schedules.
Professional development and learning. Competitive employers now provide a wide range of development opportunities for employees to stay engaged and developing in their roles. LinkedIn reported that 44 percent of people said development and career advancement opportunities were the reason they chose their current jobs. Employees seeking out companies with new ways to help their employees grow and feel empowered to keep learning inside and out of the workplace.
Diversity and inclusion. Diverse and inclusive teams have shown to help employees feel more engaged and psychologically safe. Diversity is about representing different backgrounds throughout the organization (racial, religious, socioeconomic, etc.), while inclusion is about the environment and how each person experiences the workplace. Teams can incorporate diversity and inclusion into their organizations by using bias-reducing hiring practices, offering generous parental leave, ensuring equal pay, and hosting training sessions on unconscious bias. The most important step to diversity and inclusion is building an inclusive workplace culture.
Recognition and rewards. Employee recognition is the open acknowledgement and expressed appreciation for an employee’s contributions. It’s a fast-growing trend and can increase employee engagement up to 60 percent. Companies who utilize recognition and reward programs have reduced turnover, enhanced productivity and improved morale. A recent Deloitte study found that employees who receive small, regular rewards in the form of money, points or thanks are eight times more engaged than those who receive compensation and bonuses once a year.
Healthcare Spending is on the Rise: Here’s how Employers Can Help - May 14, 2019

The U.S. healthcare system ranks last in numerous categories among other wealthy, advanced countries, according to a report released by the Commonwealth Fund last year, even though the U.S. spends the most on health care per capita.
Employer healthcare costs are expected to reflect a six percent growth in 2019, a rate that is above inflation. Expensive new medical services, escalating costs of drugs and market consolidation are driving a higher burden that typically ends up on the backs of employers. However, higher costs aren’t producing gains in consumers’ health and productivity. Interested employers can support their employees and help combat rising healthcare costs by implementing some beneficial workplace programming.
Promoting employee health and wellness is one tool employers can use to support employees and combat rising health care costs. While the jury is still out on the long-term benefits of employee wellness programs, studies show that healthy employees are happier at work. Healthier employees also keep costs low for employers sponsoring healthcare insurance. Incentivize employees to meet a health goal – or disincentivize unhealthy behaviors, such as smoking, with higher premiums.
Healthcare spending education programs are an essential tool that employers can use when cutting costs. Well-informed employees can make better decisions about their healthcare spending. Teaching your employees to use HSAs, FSAs and educating them on all options can prove invaluable. Some insurance companies offer consulting or advocacy services to help steer employees toward preventative medicine and healthy living habits.
Utilizing strategic vendor management can have a great impact on lowering costs for both employers and employees. The time and labor involved with managing healthcare plans is often the biggest burden for a company. To free up time and energy, partner with strategic benefits managers like BPA who are trusted in the business and have a proven record for successful benefits management.
A Union’s Place in Politics - May 7, 2019

Unions are often fighting on the front lines for their members, advocating for higher wages, better benefits and improved working conditions. But perhaps the biggest fight unions face is the politicians developing those polices in the first place. As new Democratic candidates step into the 2020 field, unions are finding their own place in politics and the 2020 election cycle.
Unions wield incredible influence over a wide range of policy issues. Their members care about jobs with fair wages and working conditions, keeping money in their pockets, feeding their families and securing good benefits. If a candidate wants to win the support of unions, they’ll need to step out of the beltway rhetoric and engage in the kitchen table talk most are looking for from a large field.
The large Democratic field is also amplifying workers voices and issues. Leading Democratic presidential candidates were some of the first to comment on and voice support for the Los Angeles teachers’ strike, and the Stop and Shop strikes – giving the movements a place on the national stage.
Unions also support their members by making monetary contributions to candidates willing to support common causes. Altogether, unions spent more than $2 billion on politics in 2018, according to a study by the National Institute for Labor Relations Research. Union spending was up $300 million from 2016, a presidential election year, indicating that unions are now spending more at the state and local level. Nearly a quarter of the 2018 spending, $479 billion, went directly to state politics, more than double what the Labor Research group found in the previous election cycle.
The switch comes as unions are fighting a trend by states to adopt right-to-work laws, which prohibit workers from being forced to either join a union or pay one a regular fee. Four states have adopted the laws since 2013, but a fifth one, Missouri, voted to repel such a law in 2018. The same year, a Supreme Court decision, Janus v. American Federation of State, County and Municipal Employees, effectively said that state and local public sector workers are under right-to-work protections.
Unions allow workers to band together to create one solid, unified voice when speaking to elected officials. As the 2020 election season begins to heat up, candidates willing to hear out and work with unions across the country will become top contenders. After the Supreme Court ruling in the Janus v. AFSCME case and the highly visible and systematic dismantling of 40 years of workers collective rights secured in Abood v Detroit – many commentators predicted that the Union model was in fatal drawdown. The current trends in renewed political resolve, renewed political relevance and renewed campaign contributions suggests the opposite. Far from being spent, Unions are finding ways to be at the center of the conversation – as the economic divide stretches the ethical and moral fabric of society across the globe.
Creating a Family Leave Policy that Works - April 30, 2019

The U.S. is one of the only developed countries with no paid parental leave law in place. The closest thing to parental leave law is the Family and Medical Leave Act (FMLA), which requires employers to offer up to 12 weeks of leave to employees; but FMLA doesn’t even apply to companies with under 50 employees and doesn’t guarantee the employee gets to keep their wages or salary during leave.
A lot of companies are taking it upon themselves to create their own family and medical leave policies – employees are considering benefits just as much, if not more than salary these days. Here are a few ways to create a family and medical leave policy that works for your company:
Do your research. What is your company’s budget? Be realistic about what your company can afford. With that said, consider how much turnover costs vs. a solid leave program that encourages retention and brings great talent to your company. Find out what your employees are looking for in a family or medical leave program. Speak to other companies and organizations like yours to find out what has worked and what has not. Learn from the mistakes and successes of others.
Lay a strong foundation. Build a good, strong set of benefits, not just paid leave – healthcare, retirement, etc. are important to retaining great employees. Your policy also does not have to be all or nothing. For example, start with half paid and half unpaid leave if that is what works best for your company.
Don’t be afraid to get creative. Try choosing a different name for maternity leave or paternity leave (ex. family leave). Consider innovative programs that help people based on the feedback in your research. For example, try an “off-ramping” program where employees transition work to other team members just before departing and can leave at the drop of a hat if necessary. If it fits the culture of your company, try using births as a time to celebrate family. Encourage coworkers to send cards, snacks, or drop by for visits if appropriate.
Have the policy in writing and accessible. New and existing employees should be able to find the leave policy in your handbook and maybe on your share drive or website. Let potential employees know what they have to look forward to and why they should join your company. Keep current employees with a clear and fair policy that is easy to find.
Request feedback and adjust as needed. Leave room for flexibility; the first few months of this policy may be a learning experience. Adjust the program as needs evolve and ask your employees for feedback. Find out what went well and what did not after they return from leave and adjust accordingly.
Creating a modern and fair leave policy that works for your company does not have to be a challenging undertaking. Speak with your employees to learn more about their wishes and expectations to create a program that works for you.
Spring Cleaning Cybersecurity Checklist - April 23, 2019

Though 71 percent of cybersecurity attacks are mounted on small businesses, anyone can be a victim. Below, we’ve outlined a checklist of seven items to consider:
Clearly document cybersecurity policies. Some businesses operate by word of mouth and intuition on cybersecurity, but establishing clear protocol is very important to creating a unified front. Consider including employee-focused checklists for staying safe and online trainings
Use a firewall. The first line of defense against cyber-attacks is a firewall. Be sure to research the best firewall for your company based on budget and size. Ensure employees have access to this firewall at home to protect personal and company data for remote and teleworking employees.
Establish a solid passphrase. The era of the password is long behind us. Companies and employees now must establish a unique passphrase with special characters to avoid hackers. Consider changing this passphrase every 60 to 90 days.
Use multifactor authentication. In addition to your new passphrase is the use of multifactor authentication - often a combination the passphrase and another verification (ex. code sent to a mobile device). Multifactor authentication is more difficult to hack, a login with this tool requires proof of knowledge, possession and inherence.
Trust your intuition. If an email raises red flags in your mind, it may be spam, so trust your gut on this one. Do not reply to emails or click on links that you think may be a threat to security and report it immediately. Always better safe, than sorry.
Train employees on good cyber “hygiene”. Utilize protocols and toolkits to inform and educate employees on what it is and how to practice good cyber “hygiene”. Ensure employees stay up to date and informed on the latest methods used by scammers. Cyber attackers are always evolving, so consider doing these trainings and updating information yearly.
Meet with a cybersecurity professional. Certified professionals can assist businesses with set up of cybersecurity protocols or help them bounce back after an attack. Do not be afraid to seek out help establishing solid cybersecurity policies - there is too much at risk!
Cybercriminals are getting more and more savvy every day. Keeping your employees educated and your business protected is imperative.
Reviewing the SECURE Act, RESA and how Congress plans to simplify saving for retirement - April 16, 2019

It’s no secret that America is facing a retirement crisis. One in five American adults have nothing saved for retirement or emergencies. Another 20 percent have saved 5 percent or less of their annual income. Less than a third of all Americans have saved at least 11 percent or more.
The Setting Every Community Up for Retirement Enhancement Act of 2019, or the SECURE Act, originated in the House Ways and Means Committee and is intended to address the retirement crisis in America. The SECURE Act has passed committee and is waiting on a scheduled vote on the House floor. The Senate counterpart of the SECURE Act is RESA, the Retirement Enhancement and Savings Act, which was reintroduced this month. RESA sits in the Senate Finance Committee, with no scheduled hearing thus far. Both are in the infancy of the process and could change if and when they become law.
Keeping track of these proposed changes and the difference in each bill can be daunting. BPA has broken down the major propositions in each bill and how they compare, so you can follow along as this legislation develops.
A good portion of the proposed regulations affect small businesses and small employers.
Other pieces of the legislation address issues related to non-traditional employment.
Other parts of the SECURE Act and RESA aim to change contribution and withdrawal policies.
As these two pieces of legislation work their way through their respective processes, BPA will continue to monitor changes and discuss what these changes may mean for the benefits administration industry.
The Rise of Financial Wellness as an Employee Benefit - April 10, 2019

Traditional benefits are changing. As unemployment hits a low, millennials become the prominent majority and Gen Z begins to enter the workforce, employers are reevaluating the ways they appeal to potential employees. Companies are now offering wellness benefits to sweeten the deal, and the data-backed science shows that it’s paying off.
A recent study by SHRM highlighted the fact that employers must leverage a competitive benefits package to potential employees, as benefits start to outweigh salary as a tool for recruitment and retention. A 2016 Aflac Workforce report showed that 60 percent of employees would take a job with a lower salary but great benefits, and 42 percent say a positive change or increase in benefits would persuade them to keep their current position.
To remain relevant and appealing to a changing workforce, employers are thinking outside the box and looking at the bigger picture of wellness benefits: expanding to employee financial wellness.
The student loan debt crisis has hit a whopping $1.8 trillion, and 65 percent of Americans have little to no savings. Millennials – the largest segment of the U.S. workforce - have lofty financial goals, but 43 percent have borrowed money from their parents in the last year, and 30 percent have skipped a meal to save money. There is a true issue with lack of financial literacy among this group of employees. Only 22 percent of millennials received formal financial literacy education from an employer or educational institution, and many find it too costly and low on their priority list to seek professional advisement.
As employers begin to bridge the gap through financial literacy programs as a benefit, companies are finding that physical health is just one component of a number of factors that affect overall employee wellbeing and productivity, performance and turnover. The correlation between financial stress employee health is too large to ignore. Nearly half of employees are stressed when dealing with their financial situation, resulting in more sick days, employee apathy, burnout and high turnover.
Employee financial wellness programs are beneficial to both parties. Employers put a lot of time and energy into 401(k) programs and some include matching, but 28 percent of Americans have an outstanding 401(k) loan, making the 401(k) little more than an expensive emergency fund. The most comprehensive financial wellness includes programs that teach saving for retirement, debt reduction, budgeting and goal setting - setting employees up for financial success outside of the office, and allowing them to use employer resources, such as 401(k)s, to their fullest potential. The end result reduces stress, increases employee happiness, and therefore productivity and low turnover.
Even providing a range of these benefits – including advice from a certified financial planner, help with taxes or setting up a 401(k), or any combination of those – can be invaluable to employees, and invaluable to a company.
How Unions are Shaping the Side-Gig Economy - April 3, 2019

Freelancers make up one-third of the U.S. workforce – and that number may rise to 50 percent by 2020. The Bureau of Labor and Statistics cites over 10 million contract workers without access to traditional benefits. However, unions are stepping in to fill a space otherwise unoccupied, giving new opportunities to the side-gig economy.
Growing union representation makes this type of employment more appealing to those who previously may not have considered self-employment. Many now have access to benefits through unions, as well as worker representation and protection that they cannot provide on their own. Side-gig and freelance workers are also finding community among unions where they connect, share experiences and learn in ways that many independent workers do not have access to outside of a union.
A New Way to Earn Benefits
Finding benefits as a side-gig worker, self-employed, independent contractor can be a challenge. Some unions are filling a dire need for independent contract and side-gig employees by providing portable benefits. Health care and retirement can travel from job to job with an individual, instead of being specific to one client or company. These portable benefit plans can be incredibly impactful; contract employees no longer have to depend on state health care exchanges, and the ever-changing rules and regulations of marketplace health care as Washington battles with how to handle universal health care policy, or SIMPLE IRA laws.
In addition, portable benefits are prorated, meaning that they can purchase based on hours worked, instead of one blanket price per policy. Finally, these portable benefits are universal, and they are available regardless of the working arrangement, providing access to those who may have otherwise been able to afford benefits.
Representing and Protecting
Unions are changing the side-gig economy by providing representation and protection to a subset of workers previously falling between the cracks. In the case of companies such as Uber and Airbnb, hourly “side-gig” employees were alone facing an uphill battle when asking for a livable wage, reasonable working hours and fair conditions.
The presence of unions in this new era has been key. There is now an entity on the side of workers, encouraging contract employers to pay a living wage to their employees, protect against contract nonpayment and lobby state and federal government for fair regulations affecting contract employees.
Providing Community
Unions have stepped into the side-gig economy and built community for a group of independent workers. In this community, individuals can find resources and a network to other freelancers and self-employed individuals, connecting people and ideas.
Unions also provide resources and educational programming specific to independent contractors. For example, the Freelancers’ Union provides guidance on prepping taxes, which are different for contract than traditional employees.
Progress is far from perfect, but unions have already made a big impact on the freelance and side-gig economy. Providing benefits once known by only full-time employees, quality representation and a sense of community, the recent developments by unions are charting a path for this industry.
Fair Labor in the Age of Amazon - March 2019

Lately, it seems like technology giants such as Amazon are taking over. How do unions plan on finding a symbiotic relationship with these big businesses?
Amazon met challenges in New York from the second the company announced the city for consideration of its second headquarters. The November election reinvigorated a left leaning public who opposed subsidies to be provided to Amazon, the very quiet negotiation process of the deal and the potential neighborhood impact. Protests started almost immediately, encouraging the technology and retail giant to take their new headquarters elsewhere.
The Retail, Wholesale and Department Store Union called on New York City and the state of New York to withhold subsidies (approximately $3 billion) unless Amazon established a “fair process” for its warehouse workers in the city to unionize. However, Amazon was never clear on their stance. An Amazon executive told the City Council they would not remain neutral in an organizing campaign at local facilities. Shortly following, an Amazon spokesperson released a public statement saying they “respect the rights of employees to choose to join or not join a union.”
Amazon is just one case of many run-ins between unions and tech giants.
There has been minimal union presence in technology companies to date, but as millennials become increasingly interested in joining unions, the unions must learn new ways to work with this type of industry. In addition, unions must find ways to engage independent contractors and self-employed workers; NPR reports that 1 in 5 American workers are on a contract basis, many employed by technology companies. These companies and their employees often challenge the traditional employee model and threaten previously unionized jobs in a number of sectors. For example, taxi drivers are quickly being replaced with Uber, and hotels are being replaced with Airbnb hosts and subcontracted cleaners.
It’s clear to unions that there is a role to play, but the labor movement is divided on how to work with these new tech-based companies. As in the case of Amazon HQ, do unions use their influence to force concessions, and risk ostracizing these companies altogether, or do they use their influence to take a less adversarial approach, guiding negotiations into fair compromise for both the companies, workers and unions?
The Amazon deal in NYC was a prime example of these two conflicting approaches. On one hand, allowing the building-service workers to unionize would have shown that unionization is a positive and effective way to equally allocate wages, ensure there are processes for dealing with sexual harassment and absenteeism, and create order among the workforce. Others say unionization would have made no difference, because service workers are far removed from what most other Amazon workers do, who are not unionized. Many other companies have unionized building-service workers but are otherwise not unionized.
As the trend continues, technology companies will continue to seek out headquarters in union-backed hubs across the United States. In the long term, everyone will benefit if unions and big tech can learn how to work together.
Marijuana in the Workplace - December 2018

Support for marijuana legalization reached new highs in 2017, showing that 64 percent of Americans favor legalization, and a whopping 83 percent approve of legalizing medical marijuana.
As a growing number of states legalize and tolerate marijuana use, employers are finding it increasingly difficult to reconcile their traditional zero-tolerance drug policies with new laws permitting the use of marijuana. Some have even expressed concern with violating disability discrimination laws by prohibiting such use in the workplace. For example, the Americans with Disabilities Act (ADA) prohibits covered employers from discriminating against individuals based on a disability – it even requires those employers to provide reasonable accommodations to employees with disabilities so they can perform the essential functions of their job.
Medical marijuana is often prescribed to individuals whose disabilities are typically recognized by courts under the ADA, including seizure disorders, Crohn’s disease and permanent nerve-related disorders, and in some cases, the use of medical marijuana can have a significantly positive effect on individuals’ abilities to perform major life activities. In other words, the use of medical marijuana can be essential to an employee’s ability to perform his or her job and may be the only workable accommodation for the employee.
The statute seems clear. Employers must provide reasonable accommodations for employees with disabilities to perform essential functions of their jobs.

However – Section 12114(a) of the Americans with Disabilities Act also states that “a qualified individual with a disability shall not include any employee or applicant who is currently engaging in the illegal use of drugs.” Because marijuana remains a prohibited Schedule 1 substance, courts have historically ruled that
Though marijuana prescribed by a doctor is still considered an illegal use of drugs and not covered by the Americans with Disabilities Act, that may not be the case in all states. Some have enacted anti-discrimination statutes that require employers to provide accommodations to the employee with the disability, without posing a direct threat to the health and safety of other individuals. States such as New York, Arizona, Delaware, Minnesota and Nevada prohibit employers from taking adverse action against an employee prescribed marijuana by a doctor, unless not doing so violates federal law. Even courts in Rhode Island and Massachusetts have decided that employers must in the very least attempt to accommodate those with prescriptions for medical marijuana.
This is undoubtedly a large shift from the past. Even the most progressive states – California, Oregon and Colorado – have previously held that employers do not have to accommodate medical marijuana use even if it is state law. It has become important for employers to carefully review the anti-discrimination laws in their states as it relates to medical marijuana in the workplace and consider revising their company policies. At the very least, it has become clear that many employers are not taking adverse employment action based on a positive test for marijuana should the employee have a prescription and is used in accordance with the law.
Unions Serve as Advocates for Expecting Mothers - November 2018

In addition to the physical stressors brought on by pregnancy, expecting mothers also face a wide array of tough questions before giving birth. Can she afford to take maternity leave? How much? Will, if any, of that leave be paid? Will the government help stabilize her pay during the first months of her child’s life?
The United States is the only industrialized country lacking federal law requiring a woman to be paid on maternity leave. The Family and Medical Leave Act protects a woman’s job while she’s away but does not ensure pay. Even so, this law only applies to public agencies, private sector companies with 50 or more employees, or a public or private school. Eligible employees must work for a covered employer for at least 12 months, have 1,250 hours of services in that 12-month period and work at a location where the employer has 50 employees within 75 miles.
A large part of the American population is not covered by this law – and that part is disproportionately low-income. The American Public Health Association cites that just one in four mothers take maternity leave because lack of affordability limits them from doing so. Even when employers are required by law to provide paid maternity leave, as is the case in six states and the District of Columbia, many women still choose to forego maternity leave because they cannot afford to miss out on overtime and bonus pay, or do not even realize these policies exist.
Unions, once only associated with blue-collar workers, have recently stepped in to solve the problem eluded by the U.S. government. A Vanderbilt University study found that union-represented women in the United States are 17 percent more likely to take maternity leave than women not represented by a union. The study hypothesized that a working woman’s decision to take maternity leave depends on four factors: availability, awareness, affordability, and assurance. In other words, if a woman has a paid-maternity-leave benefit available to her, she also has to be aware that the leave exists, be able to afford to take it, and be assured that she won’t risk losing hours, pay, or promotion opportunities in the long term.
Researchers also found that women with union representation tend to take leave more often than their nonunionized counterparts simply due to the presence of union representatives, workplace educators and advocates, as well as union meetings and newsletters. Simply offering a benefit does not necessarily mean it will be utilized. While the decision to take extended leave is very complex, unions help their members better understand their benefits and the options they have available. According to the Department of Labor, union-represented workers are more likely to have access to retirement plans, life and disability insurance, child-care subsidies, and health-care benefits. And in addition to helping moms take maternity leave, unions can assist workers in more understated ways: A 2014 study by the Nevada Law Journal found that when workers participate in union activities such as meetings and campaigns, they develop communication and self-advocacy skills that can pay off on the job.
The Changing Landscape for Benefits Plans

Recent actions by the Administration and Congress are changing the benefits landscape and affecting a majority of America’s workforce.
Retirement: Relaxing regulation on Multiple Employer Plans (MEPs)
Commonality and “bad apple” are two regulations that the current administration seeks to reverse, viewed by many as making MEPs difficult and expensive to manage and inaccessible for small employers, the removal of these two potential safeguards suggests a period of booming expansion in this sector, since participating employers simply need to belong to the same Chamber of Commerce. The DOL has been asked to remove the commonality requirement and explore raising the age cap for required minimum distribution of retirement accounts from 70 ½ to 72 ½, to address a workforce retiring later in life.
Another legislative action potentially affecting retirement benefits revives the Pooled Employer Plan (PEP). The Senate recently reintroduced The Retirement Enhancement and Savings Act of 2018 (RESA). Like the Executive Order, the RESA also removes the commonality rules and includes additional benefits:
With changes underway, the future of employee retirement benefits is rapidly shifting.
Healthcare: Recent Developments in Multiple Employer Welfare Arrangement (MEWA) and Association Health Plans (AHP)
The passing of the Affordable Care Act (ACA) laid the groundwork for further regulation of Multiple Employer Welfare Arrangements (MEWAs) and provided uniformity across state lines. To further dismantle the ACA, the Administration’s executive order exempts MEWAs and Association Health Plans (AHPs) from a few certain ACA regulations requiring them to provide basic essential coverage.
On the other hand, the order implements new guidelines requiring AHPs to comply with the pre-existing nondiscrimination rules currently established by the ACA. These requirements would prohibit AHPs from withholding membership based on an employee’s health, nor could the AHP require an employer or employee to pay a different premium based on health reasons. The executive order also expands AHP participation now allowing formation across state lines and through various industries
It’s evident that regulations surrounding traditional benefits programs are changing. People are continuing to work later in life and employers’ benefit plans must remain competitive and appealing. BPA will continue to dive deeper into these changes and bring members the latest updates.
Unions Lead the Charge against Opioid Addiction

The opioid epidemic continues to pummel America, taking the lives of more than 115 people in our country each day, according to the National Institute on Drug Abuse – and organized labor sits at the center of the crisis.
Though the debate rages on over the source of the opioid epidemic, which was recently declared as a national health emergency, many attribute economic despair as the driving force. Proponents of this argument include economists Anne Case and Angus Deaton at Princeton University. In a recent study, Case and Deaton credit the sharp increase in drug overdoses between 1999 and 2015 to “deaths of despair” rather than to the increased ease of obtaining opioids. According to their research, these rising rates of abuse and suicide are directly correlated with social and economic factors, including the prolonged economic decline in many regions of the U.S.
Unions Key to Economic Prosperity
Nearly every time wages have gone up in the private sector, it was because wages went up in the public sectors as a direct result of collective bargaining agreements led by unions. We’ve seen stagnation in wages since union membership began to drop in the 80’s drop. This stagnation has led to erosion of the middle class and contributed to the widening of the wage gap, which in turn is the source of many social and economic crises we’re facing in the U.S.Unfortunately, the “deunionization” trend that started 40 years ago seems to be picking up steam, with the Supreme Court's ruling against unions’ right to collect fair share fees in Janus v. AFSCME being the latest testament of this. If the trend continues, we expect economic turmoil in this country will only worsen, therefore fueling the opioid epidemic. In fact, a study released by the Illinois Economic Policy Institute estimates that annual economic activity in the U.S. will drop between $11.7 billion and $33.4 as a result of the ruling in Janus.
Unions Fight for Workers’ Wellbeing Unions’ pivotal role in the conversation surrounding opioid abuse extends far beyond improving wages and economic conditions. Unions have witnessed the detriment and destruction of opioid abuse and the toll it has taken on members and their families – and they’re not standing down as an estimated 2.4 million Americans suffer from opioid-use disorder. Rather than remaining idle, labor unions throughout the country are fighting for the wellbeing of our workforce.
Below is a glimpse into how unions are fighting back against opioid addiction:
In fact, the Allied Trades Assistance Program in Philadelphia, established by the Philadelphia Building Trades, provides addiction treatment programs that have proven highly successful. As part of this program, the union even plans to develop an online course designed to help union apprentices learn about substance abuse in the workplace, enabling them to better understand addiction and the related programs offered by the union.
Labor unions are woven into the fabric of our society, playing an essential role when it comes to ensuring the health and welfare of our nation’s workforce. If the battle against unions continues, we may find ourselves facing social and economic crises unlike anything we’ve experienced to-date.
Millennials Hold the Key to Union Revitalization

Organized labor took a major hit in June when the Supreme Court ruled against mandatory ‘fair share’ fees, which prior to Janus v. AFSCME, allowed public sector unions to collect fees from non-members who reaped the benefits of collective bargaining. This ruling was in line the union-busting trend that continues to gain momentum, despite fears of economic instability that could ignite if unions were to dissolve. Despite the onslaught of actions against unions, this is not the end. Unions now stand face a pivotal moment in history – and millennials stand at the center of the crossroads.
Millennials comprise an estimated 35 percent of American labor force participants, making them the largest generation in the U.S. labor force, according to data from the Pew Research Center. More than 55 million Millennials were employed or seeking employment in 2017, which leads the 53 million in Generation X and the 41 million Baby Boomers.
The Economic Policy Institute has found that “historically, younger workers have been less likely than older workers to be a member of union,” presenting a significant challenge. In the face of the Janus aftermath, the survival of organized labor in America now hangs on unions’ ability to recruit and retain millennial members.
We’re confident that despite the myriad of recent setbacks, unions CAN and WILL adjust.
The millennial workforce needs a collective voice, but this generation places emphasis on an entirely new set of concerns in comparison to their predecessors. If unions take note of the unique wants and needs of this rapidly evolving workforce, organized labor will thrive for decades to come.
The “Traditional” Workplace Becomes Obsolete
The millennial workforce has made the single job, single employer workforce of our parent’s generation obsolete. According to a survey spearheaded by economists Lawrence Katz of Harvard University and Alan Krueger at Princeton University, the percentage of Americans workers with “alternative” work arrangements leapt from 10.7 percent in 2005 to nearly 16 percent by 2015. The proportion of workers engaged in alternative work – which encompasses the “gig economy,” contract labor and freelancing, as well as other non-conventional work arrangements – will continue to climb.Participation in Taft-Hartley Plans Depend on Younger Population of ‘Actives’
It is crucial that unions appeal to and enroll as many millennials as possible. This will likely require ‘out of the box’ thinking when engaging in the collective bargaining process with employers in order to make benefits and enrollment opportunities relevant to a younger demographic. Millennials aren’t just thinking about investment, they’re concerned with homeownership, raising a family and everything in between. These things must come under consideration when entering into collective bargaining negotiations and remembering to take a holistic approach is imperative.For example, a millennial worker in today’s modern world is likely facing high student debt, all while looking to purchase a home and save for retirement. To fulfill this need, potential benefits may include tuition repayment programs or home buying assistance. On the other side of things, many millennial women are focusing more heavily on career development and in turn postponing building a family until later in life. To appease this growing trend, some progressive companies are choosing to offer elective fertility preservation as an optional benefit.
It's not just about providing options for retirement saving. It’s about analyzing the current environment and catering to the broad needs of a generation. Their retirement planning must reflect these needs and give them a one stop shop to plan, invest, monitor and control their whole financial picture at the click of a button. A comprehensive approach to money management, as well as placing a heightened focus on incorporating financial education programs is key.
Unions should take note of and consider turning to the latest benefits technology, which now allows:
Beyond the software, unions must turn to technology for communicating with current and potential members. Leveraging social media platforms and using them to engage with prospective members is certainly a necessity in recruiting new members in today’s environment.
A new, inspired, quick-to-move workforce is in play. The millennial group – anyone 36 years of age and below – will be the driving force of a new American age. They have the same natural and instinctive yearning to belong to a group – a club – rich in resources and beneficial to their common goals, just as their forebears from earlier generations. It is time to offer them not only what we have, but what they want. A surge in union strength might be more than a rescue of the middle class, it might be a moral imperative.
BPA Talks with NPR's Nina Totenberg on Impact of SCOTUS Decision on Fair Share Fees

Shortly after the Supreme Court issued its 5-4 decision in Janus v. AFSCME, BPA Executive Vice President Zane Dalal spoke with NPR's legal affairs correspondent Nina Totenberg. Nina is an award-winning journalist who has covered the Supreme Court for NPR’s “All Things Considered” throughout the past four decades.
Nina reached out to several experts for commentary on this ruling. She was particularly interested in hearing from BPA’s leadership team based on the company’s 70 years of experience partnering with union trustees to administer the Retirement and Health & Welfare benefits of Southern Californians.
This NPR interview focused on four key themes: first amendment rights, the strength of collective bargaining, potential ripple effects of the case, and hope for the future of organized labor.
Here’s a recap of the commentary Zane shared with NPR, as well as a few added insights reserved for our valued newsletter subscribers.
- 1. The heart of the case: First amendment rights
- 2. Ripple effect on social and economic landscape
- 3. Strength of collective bargaining
- 4. Hope for revitalization of labor unions
NPR Commentary
On mandatory fair share fees and nonmembers: “In the public sector, irrespective of if they (employees) pay a fee or not, they still get the benefits,” said Zane. That’s the law in most states where the ‘fair share’ fee exists. He continues to say that nonmembers who do not pay the union ‘fair share’ fee are “not paying a fair fee for services rendered.”
Additional Insights from BPA
Not paying ‘fair share’ fees for these services rendered based on first amendment principles is flawed. The same logic would allow you to refuse to pay your federal taxes because you feel your first amendment rights are violated during an administration that you didn’t vote for, and/or with whose policies you don’t agree.
As some have pointed out – not least of all the attorney for AFSCME – by ruling on this as a first amendment issue, the decision has propelled the right to collectively bargain from an adjunct construct of labor law to a constitutional right. Many on the GOP side would have preferred not to have opened this particular Pandora’s Box.
NPR commentary
On the ruling’s implications for employee benefit plans: “We must connect benefits with wider issues at play – erosion of the middle class leads to pervasive societal problems of homelessness, drug addiction, the opioid crisis, the skyrocketing cost of healthcare and a myriad other issues ripping at the fabric of who we are as a nation,” said Zane. “If we don’t see these trends as connected, we are misunderstanding the root causes of the problems we wish to address, and whatever we do will be ‘lip service.’”
Additional Insights from BPA
The ‘union made’ middle class that was once the bulwarks of a manufacturing-based economy supported our country’s ‘economic engine,’ which played an integral role in distinguishing America’s superpower status.
Within the past two decades, this middle class has been steadily eroded, resulting in the widening wealth gap and the dismantling of fair labor practices. This is connected to the loss of fair paying jobs, which is directly correlated with a drop in organized labor activity. It is vital we recognize the root of these problems in order to respond appropriately.
NPR commentary
"Wherever there’s a collective voice, we see a stronger workforce,” said Zane. He continued the conversation by emphasizing the power of a collective voice – alluding to the case filed by 17 States Attorneys General against the administration, precisely because there is strength in numbers.
Additional Insights from BPA
A historical view of our society and the American economy brings into stark relief the insidious nature of dismantling the strength of the unions. Historically, wage increases that result from unions’ collective bargaining activity ripple down to the private sector. Without public sector increases initiated by unions, wage stagnation in the private sector would prevail. The recent Public Teachers protests in several states, typically led by those without the ‘fair fee’ arrangement, point to this unfair wage discrimination – this ruling now heightens their plight.
NPR Recap
When asked what’s next for unions, Zane delivered a powerful message: “Unions will adjust.” He communicated to Nina his belief that unions will prevail. He highlights the vital role unions play in our society and their perseverance. What will lead the change? According to Zane the “millennial workforce may need a collective voice to face an entirely new set of challenges” and “unions may give them this collective voice.” He goes on to highlight potential benefits including tuition repayment programs or home buying assistance.
Additional Insights from BPA
Reversing Abood v. Detroit will nullify 41 years of established labor law and alter the governance of our workforce, potentially invalidating thousands of regulations. Therefore, the damage to the collective voice of millions of hardworking Americans will take not only some adjustment, but a reorganization of will and strength to fight back. However, organized labor is an ancient construct – from stonemasons of medieval cathedral building to the mercantile guilds of the renaissance. The idea of a collective voice has been a part of the work force for over a thousand years, and it is here to stay.
We have been following Janus v. ASFME since the Court agreed to take the case. If you are interested in learning more, follow the links below to read more BPA coverage of the case.
BPA Tells SHRM ‘Deunionization’ to Blame for Wage Stagnation

This week, the Society for Human Resource Management (SHRM) posed the question: "Where’s the Wage Growth?" Jobs reports show we’re in a tight labor market, which according to economists should mean wage gains. When SHRM’s Stephen Miller reviewed recent pay data, he found that actual wage increases are far from reaching economists’ expectations for the current labor market and turned to the experts for answers.
BPA Executive Vice President Zane Dalal attributes today’s wage stagnation to the declining of unions. "We've seen stagnation in wages since union membership began to drop in the 1980s," Zane told SHRM.He continued to state that Wednesday’s Supreme Court ruling in Janus v. ASFME – which overturned the long-standing precedent allowing unions to collect fees from nonmembers who benefit from collective bargaining activity (such as in the form of higher wages and better benefits) – may further hinder wage growth. "Nearly every time wages have gone up in the private sector, it was because wages went up in the public sector as a direct result of collective bargaining agreements led by unions," Zane stated.
Click here to read the full article, “Where's the Wage Growth?” in SHRM’s online edition.
BPA is disappointed in the Supreme Court’s decision in the Janus case and fear it will have profound ramifications, from both an economic and social standpoint. Unions are designed to give a voice to the American working class and have been the glue holding together the US economy for more than 70 years. This watershed ruling plays into the union-busting trend gaining momentum throughout the country and has the potential to disrupt the future of the American workforce and create economic instability.
To learn more about BPA’s take on Janus v. ASFME, you can read our recap of Zane’s interview with NPR following the ruling. For background on this case, we encourage you to check out Part I and Part II of our blog series “Supreme Court Ruling in Janus v. AFSCME to Impact Organized Labor.”
Benefits Plans, Third Party Administrators and Security

BPA’s CFO, Hormazd Dalal, recently authored the article “Benefit Plans and Cybersecurity Threats,” which will be included in the May edition of Benefits Magazine, the official publication of the International Foundation of Employee Benefit Plans. Within the article there is a brief overview of audits and controls for third party benefits administrators. Here we are taking a deeper dive into the history of these standards and the importance of undergoing audits and exams.
Regulatory Evolution of Audits and Controls
For decades the American Institute of Certified Public Accountants (AICPA) has been the country’s leading authority on controls and served as an independent auditor to ensure third parties involved the financial reporting of their customers are fulfilling their obligation to protect sensitive information.
Since its initial Statement on Auditing Procedure (SAP) in 1939, the AICPA has issued a slew of statements and standards relating to internal controls, impact of information technology on a statement audit, and on service organizations.
- Below are a few relatively recent issuances:
- Statement on Auditing Standards 70 (SAS 70) 1992: A widely recognized standard that helps service organizations to evaluate their control objectives and activities, including those pertaining to information technology and related processes. The Service Auditors Examination was used as a means of determining whether or not companies were meeting SAS 70 requirements, and was mandatory in generating an SAS Report.
- Statement on Standards for Attestation Engagements 16 (SSAE 16), 2011: One of the most important factors of the SSAE process is that it requires an organization to provide a “management assertion of its procedures” in advance of controls and audits being conducted. This ensures that the auditors check the actual efficacy of working protocols and don’t get diverted into a grey area that may fail to provide real results. Do not short change this procedure. It is recommended to subject every internal procedure – no matter how small – to an external audit. If you are undertaking these audits for the first time, it is better to fix a problem than to get a shining report.
- Statement on Standards for Attestation Engagements 18 (SSAE 18), 2017: The SSAE 18 standard expands on the SSAE to require that sub services organizations be identified, described and monitored regularly. Additionally it requires a risk assessment, and in turn, requires regular review of the controls. SSAE 18 is the standard used for System and Organization Controls 2 (SOC 2) reports and examinations.
- If your firm is directly involved with transacting monies on behalf of clients, even if indirect, you have a duty to ensure the policies and controls you have in place are effective and secure.
- It is better to be proactive than reactive. Rather than wait for a client to inquire into the firm’s sureness and security, undergo an external evaluation so you know the firm is properly conducting business – and if there’s a problem, you can get out ahead of it.
- If you participate in the SOC certification program, you can rest assured in knowing your firm’s controls are under review on an ongoing basis – this is not a one-time event.
- The SOC certification distinguishes the firm from competitors, as you can confidently assure current and former clients you are upholding your fiduciary responsibilities.
SAS 70 audits have run their course, and though some firms still have these standards in place, they have largely been replaced by the recent SSAE 16 and 18.
Introduction of SSAE brought the audit standard in line with the international protocols set in the ISAE 3402. SSAE 16 is the standard used for System and Organization Controls 1 (SOC 1) reports and examinations.
There are many benefits and improvements to the new standards and, typical of how quickly this area is changing and redefining itself, SSAE 16 introduced in 2011 is already superseded by SSAE 18 – the standard since May 2017.
In contrast to SOC 1, SOC 2 attestations exercise vigilance over a wider area of controls and over a prescribed period of time to ensure fidelity. When going through the SOC 2 controls audit period, don’t forget to share the goals and aspirations with your workforce. Your staff are the first and last stand in a controlled environment, and therefore in meeting high standards of security.
Remember to keep the end goal in mind in terms of AICPA standards and reports – don’t consider them publicity ventures. This provides a real way to judge whether the procedures and protocols you believe to be tried and true are actually effective. Adjudicating one’s own systems is a critical endeavor and the overall value of the organization depends upon it.
- Why undergo a SSAE/SOC examination?
If you have any questions regarding these audits and controls, please send us an email. Our email address is info@bpabenefits.com.
Benefit Plans and Cybersecurity Threats: Controls Outweigh Technology

The risk of cyberattack strikes fear into organizations around the world...
The article also can be found here on IFEBP's website.
Part II: Supreme Court Ruling in Janus v. AFSCME to Impact Organized Labor

The Supreme Court’s impending decision in Janus v. AFSCME is top-of-mind for unions, employers with an organized workforce and the third-parties serving unionized workers – including our team at BPA.
In Part I of this blog series, we provided background information key to understanding the case brought to the Supreme Court on behalf of Mark Janus, a public employee in Illinois. But understanding the history of the case and past precedent is only the first step in understanding the potential impact of the ruling.
The death of Justice Scalia resulted in a deadlock when the High Court reviewed a similar case involving non-unionized public school teachers in California who argued mandatory union fees violated their First Amendment rights (Friedrichs v. California Teachers Association, 2016). However, the confirmation of President Trump’s conservative Supreme Court nominee, Neil Gorsuch, is largely expected to tip the scale in the Janus case – many experts anticipate Mark Janus will prevail in a 5-4 decision.
Union Membership Set to Drop if Janus Prevails
If fair-share fees are not required, union membership is expected to drop as workers become less incentivized to join. This would lead to a drastic decline in union revenue, and therefore result in shrinking budgets. Though the Janus case focuses on organized labor within the public sector, its ripple effects will likely have profound repercussions in the private sector as well – already facing historical lows in terms of membership.Unions were created to serve the working class and represent their best interests at the negotiating table with employers. The primary function of unions is to give a voice to workers whose voices would not likely be heard otherwise. Historically, the effects of these talks result in wage increases, improvement in working conditions, and more robust benefits packages, which include healthcare coverage, retirement plans and more.
The effects of the Janus case are numerous. If the Supreme Court rules in favor of Janus, it will be much harder for the public sector to unionize, recruit new members and retain existing members.
BPA is here to help our clients navigate the complexities of benefits plans as the regulatory landscape evolves.
Part I: Supreme Court Ruling in Janus v. AFSCME to Impact Organized Labor

Labor unions and employers with an organized labor force anxiously await the Supreme Court’s ruling in Janus v. American Federation of State, County and Municipal Employees, set to come down early this summer. If Janus prevails, which many believe to be the likely outcome, this ruling is set to have wide-spread implications for union membership, and therefore collective bargaining at large.
However, before we dive into the potential impact of the ruling, it is important to understand the premise of the case, past precedent and who may be affected when the ruling comes down.
For those of you familiar with the case, jump to Part II of this blog series for our analysis of how Janus v. AFSCME Council 31 may impact unions, employers and the American workforce.
Background on Janus v. AFSCME
Mark Janus, a child support specialist for the Illinois Department of Healthcare and Family Services who is not a union member, is arguing that mandatory union fees violated his First Amendment rights by requiring him to subsidize political views he does not support.
Though Janus is not a union member, in Illinois and more than 21 other states, workers are required to pay “fair-share” fees, regardless of membership, as they still reap the benefits of union’s collective bargaining activities. This includes union negotiation on matters such as workplace conditions, pay and benefits. Workers who do not belong to unions are not required to contribute to a union's political lobbying, support of political candidates, or other political activities. However, Janus asserts that in paying these mandatory fees he is being forced to contribute to the union's political activities despite his opposing views, thus violating his First Amendment rights.
This challenges precedent set in 1977 by the ruling of Abood v. Detroit Board of Education. In this 40-year-old case, the Court ruled in favor of forced dues, stating that workers who benefit from union representation should be required to pay their fair share.
According to the Grant for Certiorari, Abood has been challenged twice in the past five years and the Court has contemplated whether or not “it is constitutional for a government to force its employees to pay agency fees to an exclusive representative for speaking and contracting with the government over policies that affect their profession.” It goes on to state the underlying question in this case: “Should Abood be overruled and public sector agency fee arrangements declared unconstitutional under the First Amendment?”
- Terms to understand
- Fair-share fees: Mandatory fees from non-union workers that cover the costs of the union's collective bargaining activities
- Free-rider: A worker who benefits from a union's collective bargaining agreements, but does not pay union fees
- Right-to-work: The right for employees to decline union membership
This case will directly impact public sector unions in right-to-work states, which represent an estimated five million employees in the public sector – ranging from teachers to civil servants.
2018 Regulation Part 2: Joint-Employment Ruling, Paid Leave and Overtime

Employers, union trustees and third party administrators have the best intentions when it comes to managing employee benefits, but many face challenges in terms of staying apprised of the latest legislation in today's complex and fast-paced regulatory landscape. With the new year in full swing, we are here to help guide employers and trustees through the latest developments.
Here are the top three new developments you should know now to help you navigate the complexities of benefits management in 2018, while also maintaining a sustainable business model.
Browning-Ferris decision determining the definition of joint-employment status reversed.
In 2015, the National Labor Relations Board (NLRB or “the Board”) issued a decision in the Browning-Ferris Industries case that upended the long-standing standards of the joint-employment test, throwing many into a tailspin, most notably franchises and employers working with third-party.
Upon issuance of the decision, the Board mandated that any party with indirect control over an employee was responsible for ensuring proper pay and workplace conditions and could held liable for any wrongdoing, as well as subject to negotiations with labor unions, regardless of whether they played part in such practices. For example, if a franchisee did not pay an employee overtime for hours worked in excess of 40, the corporate franchise could be held liable. The same was true of an employer who used a temp worker, despite not having knowledge of the temp agency's pay practices. This reversed the traditional standard in the joint-employment test, which mandated the entity must have direct control over an employee's workplace conditions and pay practices in order to be deemed an employer.
However, in December 2017, the Board reinstated the status quo in its 3-2 decision in Hy-Brand Industrial Contractors. Returning to tradition, only entities with direct control over employees pay and workplace conditions may be deemed as “employers.”
Paid-time off initiatives push forward.
Federal Initiative
Included in the new tax plan is a tax credit for companies that offer employees two or more weeks of paid family or medical leave a year. This is available if three requirements are met: 1. The employee must not earn more than $72,000 a year, 2. The company must cover 50 percent or more of employees' earnings, and 3. The employee has been with the company for at least a year. Companies can receive 12.5 percent of the amount paid in tax credits at the 50 percent level, which increases on a sliding scale if the company covers more than 50 percent of employees’ earnings.
Currently, companies must allow employees up to 12 weeks of unpaid time off under the Family and Medical Leave Act (FMLA). This new program was designed to test the effectiveness of a paid time off approach and is set to end after 2019.
State legislation
On January 1, New York joined California, New Jersey and Rhode Island in requiring employers offer employees paid family leave. New York employers in the private sector must now provide up to eight weeks if paid leave to employees who need time off to care for a sick child or bond with a new baby, take care of a close relative with a serious illness or injury, or assist loved ones during a family member's military deployment.
This is the country's most expansive legislation on family leave. This year, employers must provide up to eight weeks of paid leave, offering at least 50 percent of employees' average earnings, up to a weekly cap of $652. This is part of a multi-tiered phase in program, which, when complete, will require employers offer 12 weeks and pay at least two-thirds of employees' average weekly earnings.
Washington state employers are required to offer paid sick leave to non-exempt employees covered by state minimum wage laws, as of January 1. Washington employees, including seasonal and part-time workers, are entitled to one hour of paid sick leave for every 40 worked. This must be provided to employees beginning on their 90th calendar day worked, and employers must allow employees to carry over up to 40 hours of unused leave into the next calendar year.
As of February 11, many Maryland employers are now required to provide employees with paid sick leave. Employers with 15 or more employees must offer one hour of paid sick leave for every 30 worked – employers have the option of frontloading 40 hours at the beginning of the year or offering on an accrual basis. Maryland employers with fewer than 15 employees must provide the same amount of unpaid leave.
In addition to state regulation, many municipalities around the country have enacted similar laws. Employers, unions and TPAs should review local and state legislation to ensure compliance.
Department of Labor halts advancement of overtime rule, but revisions to current threshold expected in late-2018.
Days before a drastic increase to the overtime pay requirement was set to take effect, a Texas judge hit the brakes and delayed the rule's December 1, 2016 implementation. The rule would have significantly increased the number of employees eligible for overtime pay by requiring employees make a minimum of $47,476 annually to be exempt from overtime, up from the current $23,660.
The DOL originally planned to battle out all objections in court, but decided to drop its defense in 2017. However, a new and revised proposal to increase the current salary threshold is expected in October of this year, according to the DOL's fall regulatory agenda.
Regulations impacting the benefits landscape are rapidly evolving, and those responsible for employee benefits programs must keep up or risk a cumbersome legal battle. When designing benefits packages, be sure to always research current and upcoming regulations on the federal, state and local levels.
2018 Regulation Part 1: Health Care Reform on the Horizon

Trump Administration Targets Obama-Era Regs
It's no secret that the Trump administration opposes regulatory overreach. Completing a year in office, President Trump has already made good on his campaign pledge to dismantle hundreds of Obama-era regulations. As he often states, President Trump believes in shrinking the government's footprint while allowing more latitude for the private sector to organically boost the American business engine. Toward this end, his administration has halted or delayed a slew of regulations across industries – from energy and environmental protection to financial services and health care.
Trump Administration Pushes for Sea of Change in Health Care, Lawmakers Divided
Important areas impacted by the Administration’s deregulatory trend include lesser known rules as well as signature legislative changes under the prior administration, including the Affordable Care Act (ACA).
On the health care front, Trump has proposed scrapping government-funded, cost-sharing reduction (CSR) payments to insurance companies. These payments help reduce employee insurance co-pays and deductibles for low-to-moderate income individuals. Nearly 60 percent of benefits plan enrollees qualified for CSRs this year, according to estimates from the Department of Health and Human Services.
Eliminating these subsidies would significantly change the insurance landscape in terms of carriers' ability to compete in the ACA marketplace and workers’ access to coverage. Not only do critics contend the move would increase ACA premiums by as much as 20 percent, but some says it also would cause rates to soar, since many insurers plan to hike rates to compensate for eliminated subsidies. On the other hand, the White House views CSRs as an unlawful means of propping up the "broken" insurance industry with taxpayer dollars.
Compromise Proposed
Lawmakers from both parties have pushed back on a wholesale repeal of the payments amid lawsuits filed by state attorneys general and other involved parties — legal wrangling is expected to continue for some time. However, bipartisan constituents are poised to bring relief on the CSR issue sooner rather than later in order to help stabilize health insurance markets now rattled by the controversy.
In late October, a compromise was proposed in the form of The Bipartisan Health Care Stabilization Act of 2017. The Congressional Budget Office (CBO) estimates the bill could cut the federal deficit by $3.8 billion in the coming decade. The bill protects CSR subsidies through 2019 and paves the way for a broader tier of plans exempt from the ACA requirements, such as pooled risk plans through associations of small employers, as well as greater use of short-term and "catastrophic coverage" plans.
New Tax Bill Repeals ACA Individual Mandate
President Trump signed the GOP tax bill into law before breaking for the holidays on December 22. The tax bill’s most significant regulatory change in terms of benefits is the repeal of the ACA’s individual mandate, meaning individuals will no longer be penalized if they choose not to have insurance. However, the tax bill does not repeal the employer mandate, which requires employers pay an assessed taxable penalty under the ACA for not providing fair market place health coverage to their workforce (more than 50 employees), thus spelling trouble for employers.
The intent of the individual mandate was to increase the number of healthy individuals in the insurance marketplace, with the idea that the healthy could subsidize sick. Repealing the individual mandate without repealing the employer mandate likely will open a can of warms and cause trouble for employers. If healthy individuals opt out of coverage without penalty, employer premiums are likely to spike, which is not a sustainable option.
With this in mind, we expect repeal of the employer mandate is not far behind. However, before making any changes to health plans, plan sponsors should keep in mind that the enforcement of the change may not take immediate effect. And further, it is important to look into local and state regulations prior to making modifications. It is very likely that states which a form of Exchanges were successfully put in operation, especially California, will close the gap to keep some form of Covered California functioning and viable.
Additionally, it is important to remember that what is done by one administration can be undone by successive acts of Congress. Only time will tell what version of the health care plan will remain.
The deregulatory trend under the Trump administration has myriad implications for benefits plans. Plan administrators are watching these developments closely to help keep benefits plan professionals, union representatives and workers informed.
Integrated Web-Based Content Facilitates Plan Participation

by Lance Phillips | LinkedIn
New technology-enabled enrollment systems are alleviating the administrative burden on employers while streamlining the election process for employees. Above and beyond these benefits, automated enrollment solutions help educate employees about the benefits to which they are entitled, and make the process less stressful. Doing so can go a long way to boosting benefits plan participation.
A growing number of employers and plan administrators are investing in automated enrollment solutions to deliver a more engaging benefits plan service and support model. In the last five years, new technology-powered solutions have gained increased adoption. The more advanced solutions are tailored to the employer and its workforce. For instance, proprietary and carrier-provided auto-enrollment systems can be populated with employee enrollment data and plan selections.
In the absence of these new enrollment platforms, employees easily can be overwhelmed in the benefits decision-making process given the plethora of available insurance and financial products, according to a 2008 study by Yale University. Employees also are often reluctant to go online to buy, particularly in the absence of a source of answers to questions they may have.
An Educated Consumer: Your Best Benefits Plan Consumer
Automated enrollment platforms make it easier to educate employees about the benefits available to them. For instance, they explain the benefits products offered by the employer in plain English. Especially valuable during open-enrollment times, automated platforms deliver answers to questions more efficiently than an employer could offer on a one-to-one basis. Indeed, technology eases the enrollment process by giving employees access to benefits information at their fingertips.
Some carriers offer their rates, underwriting guidelines and benefits options online while employer-tailored health and welfare plan benefits instantly can be reviewed. Auto-enrollment can also encourage investment plan participation by delivering web-based access to information and automated re-enrollment reminders for plans that are selected for a specific workforce.
To support employees who have questions about their unique circumstances, many employers supplement their online knowledge base with access to a live help desk or integrated chat tools. Such platforms can provide training and technical support on a range of topics, such as eligibility rules that can otherwise be dauntingly complex. Online communications can be simplified and personalized, enabling employers to interact with employees to promote loyalty and engagement.
Instead of delivering generic benefits information to employees, companies can set up their platforms to deliver customized communications, including reminders employees can put on their calendars with the push of a button, automatically nudging them when open enrollment is approaching.
Employers can also leverage automated enrollment systems to become "choice architects" — a term coined in the Yale study — effectively reducing the deluge of benefits options to a handful of those that match their employee needs and demographic profile. Science has shown that people can be paralyzed when presented with too many options. Enrollment platforms get around this problem by helping to simplify and streamline benefits plan decision-making for employees.
Mining Data to Improve Employer Benefits Plans
In addition, enrollment technologies gather data that allow employers to analyze which employees enroll in which benefits based on variables such as age, income, gender and location. Data tracking help reveal meaningful employee patterns. A graphical "heat map" based on such patterns enables employers to design and present plan choices that are suitable to their workforce.
Employees appreciate other advantages that auto-enrollment solutions provide. According to a 2013 study by employee benefits products and services provider Unum, a lack of knowledge and awareness can curtail employee access to vital benefits like disability insurance; and fully 85 percent of respondents believe employers should automatically enroll new employees in disability insurance to help avoid inadvertent disruption or lack of such benefits, allowing them to opt out if they choose.
Given advances in benefits plan technology, employers of all sizes have a range of options that are facilitating and improving enrollment benefits plan administration. By easing consumer decision-making, employers have more sophisticated tools to increase benefits plan participation. Enrollment technologies are a new means of encouraging employees to consider the benefits options that are right for their families while removing stress and complexity from the decision-making process.
Enrollment Technologies 101

by Lance Phillips | LinkedIn
Technology powered enrollment platforms are replacing manual methods to make it more efficient for businesses to enroll employees in retirement, health and welfare benefits plans. Along with other advantages, we have seen a drastic uptick in employee enrollment technologies used to facilitate employee participation in benefit plans.
For instance, many plan sponsors are electing to shift from manual enrollment to auto-enrollment, meaning employees are automatically re-enrolled into coverage without needing to fill out any additional paperwork. However, auto-enrollment does come with an opt-out provision.
Surveys show that employees increasingly trust employers to offer appropriate plan options for them, thus they are more open to auto-enrollment than ever before. In fact, according to a recent study conducted by the Consumer Federation of America on long term disability insurance, 85 percent of disability beneficiaries agreed that employers should auto-enroll all new employees in disability insurance. Employees understand that auto enrollment helps them avoid inadvertent disruption of vital benefits like disability insurance.
These interrelated trends reverse the longstanding and purportedly less efficient alternative of manual employee elections, such as the selection of health care plans during open enrollment. Additionally, auto-enrollment may encourage plan participants to invest early and more often. Web-based technologies facilitate employees' retirement planning by delivering integrated investment plan information – specific to the employee – along with automated re-enrollment reminders.
Technology not only eases the enrollment process for employees by ensuring they have all needed information at their fingertips, but it also benefits employers. Transitioning from pen and paper to electronic processes reduces the administrative burden on employers, while increasing accuracy and transparency during the enrollment process.
- Auto-Enrollment Benefits at a Glance
- Expedites the enrollment process through use of technology, offloading the traditional administrative burdens
- 24x7 connectivity enables fluid communication between employees and human resource departments, through tools such as autoresponders
- Empowers data tracking and mining of information so employers can identify meaningful employee patterns
- Improves quality of support through employer-specific services, maintenance and reporting
- Increases processing accuracy via standardized rule-based processes and forms
- Allows for secure online data imports and exports, providing a richer user experience
As auto-enrollment continues to pick up speed, we are seeing the debut of more and more technologies focused on automation and employee engagement. Some systems even offer a tailored approach based on the needs of individual firms and their employees – including setting up carrier relationships with enrollment data, designing plan selections and integrating this data with enrollment platforms. Some systems even go a step further in offering ancillary web-based services connecting carriers to the platform, making for an even more robust employee experience.
For instance, some carriers offer their rates, underwriting guidelines and benefits options online, reducing the need for employees to turn elsewhere to seek answers to questions about plans offered.
Additionally, these tech-centric platforms can provide training and technical support on a range of topics, such as eligibility rules that can be complex and subject to change. Online communications can be personalized to employees, enabling employers to interact with their workforce in ways that promote loyalty, serving as tangible evidence that a business is invested in the wellbeing of its employees beyond the workday.
An auto-enrollment system enables firms and their employees to derive all of these benefits without disrupting day-to-day operations. Added benefits offered on many of these systems include: system trainings; standardized enrollment forms and communications templates, such as email autoresponders; and best practices, tips and tools geared toward promoting user satisfaction.
Enrolling in benefits plans can be stressful for employees – especially knowing that health care deductibles may soon be on the rise. Many employers are shifting from full-coverage to high-deductible plans, with employees absorbing more out-of-pocket expenses than ever before. The multitude of plan options and continuous changes combined with the transfer of more costs to employees can be overwhelming.
Implementing automated-enrollment solutions demonstrates to the workforce that employers are actively working to remove some of that stress by prioritizing employees’ needs. Plan sponsors who adopt technology powered benefits platforms not only can facilitate and ease the plan selection process for employees, but they also have the ability to empower employee engagement at unprecedented rates.
If you are interested in learning more on the topic, we will take a deeper dive into enrollment technologies in our next blog post. Stay tuned!
10 Ways to Manage Responsibilities with Terminated Vested Participants

As many plan sponsors already know...
This article originally written for and appeared in Benefits Magazine.
What Individual Mandate Repeal Means for Employers

Zane Dalal, executive vice president of BPA, was quoted in the article “What Individual Mandate Repeal Means for Employers” on the Society for Human Resource Management’s (SHRM) website. He weighed in on how the repeal of the ACA mandate requiring individuals pay a penalty for opting out of health care coverage may impact employers – highlighting how it is likely to affect premiums.
"If healthy individuals opt out of coverage without penalty, employer premiums are likely to spike, and overall, this is an unsustainable option," said Dalal. He continued to explain that many in the benefits community believe repeal of the employer mandate is not far behind.
Why Outsource Benefit Programs Administration?

Outsourcing benefit programs administration to competent third party administrators (TPAs) is an increasingly common and prudent option for single and multi-employer trust funds for a host of reasons.
Foremost among them, the specialized skills needed to administer benefit programs – everything from books and records as well as cash management services to health and retirement services – are essential given today's challenging and risk-averse business climate.
The varied nature of benefit programs requires expert professionals who are trained and adept at managing them. TPAs serving many clients amass a depth of knowledge to support even the most complex programs. With the outsourced administration model, funds essentially purchase the business acumen of the TPA along with the cost benefits of services that are shared across the provider’s client base. Outsourcing avails a broader subject matter knowledge than trustees typically have in-house.
Equally compelling is the drive to contain the costs associated with benefit programs management. A TPA that serves several plans can pass along to clients the cost benefits of the shared service model along with the expertise earned over years or even decades of focusing exclusively on service provision.
Benefits Derived as a New Model Emerges
The outsourced administration model has gained momentum in recent years as trustees aim to contain costs while improving service levels. Indeed, a primary driver for outsourcing to a third party is the economic benefit. By outsourcing, funds can avoid the cost of hiring qualified personnel in-house as well as purchasing software, systems and other resources needed to administer plan benefits.
Ongoing cost benefits include the ability to gain access to the outsourcer’s skilled professionals and continuously updated software and systems. Leading outsourcers continually train their personnel and update their service platforms to maintain a competitive edge—at no cost to their clients. By relying on a TPA's specialized staff, services and solutions, program trustees can stay focused on core client-facing issues instead of the nuts and bolts of administering benefits programs.
Flexibility of Scope and Scale
By outsourcing, clients can also add or remove services much more easily as their needs evolve. TPAs serving a variegated client base offer a wide range of services. This gives clients the flexibility to scale to different service packages without having to invest directly in new infrastructure or staffing support.
Especially for small or medium sized entities, making such direct investments is a costly and inefficient commitment. On the contrary, any and all services a TPA offers are available to clients as their needs change, providing a more effective model that is flexible enough to fit benefit programs of any size.
Alignment of Business Drivers and Long-term Motivators
By leveraging a TPA’s expertise and solutions, clients can reduce their investment in technology, operations and product development while enhancing service since leading outsourcers offer an array of solutions that are continually enhanced. In addition to the benefits of service scalability and cost-containment, TPA’s long-term business drivers are fundamentally aligned with their clients. TPAs that meet service level standards and commitments are rewarded with client loyalty and referral.
TPAs and clients are equally motivated to derive increased levels of cost-efficiency and service excellence.
The best TPAs understand the value of client trust, and they take every measure to retain that trust. This includes maintaining the dedicated staff, intellectual capital, technological fortitude, and vision to stay focused on delivering the highest possible levels of service.
The Federal Government and Legal Compliance
Because of the way benefit plans must be devised, legally written and operated, they are the purview of the Federal Government. Multiple Federal Statutes that safeguard members and their access to benefits have been enacted over several decades. Participant and benefit protections under the Employee Retirement Income Security Act 1974 (ERISA), the Pension Protection Act 2006 (PPA), the Health Insurance Portability and Accountability Act 1996 (HIPAA), and a host of additional regulations, are constantly amended and updated – almost as often as Congress convenes.
The onus on compliance with these regulations is a heavy one. This presents a significant challenge to plan sponsors. A challenge they would prefer to delegate to professional administrators.
TPAs, because of their shared knowledge across the industry and their long chronological experience, are best suited to handle regulatory compliance, the multiple facets of which are present whether or not the plan is small or large. Many mid-size to smaller plans find themselves ‘snowed under’ with regulatory burdens, without expert TPA services. The outsourced model is a win-win business model because the TPA continues to hone its capabilities to remain competitive while clients reap the benefits of cost-reduction and the provider's expertise.
Article originally appeared in SHRM
Age of Anxiety

Stereotypes notwithstanding, millennial workers are actively saving for retirement. But many still struggle with fear and ignorance in managing their 401(k) accounts. Experts -- and millennials themselves -- say employers can help.
by Jack Robinson
Fred Thiele recalls a 22-year-old employee approaching him about a problem with her 401(k) account. She had hit the IRS annual limit for contributions, which currently is $18,000. Though her retirement was at least four decades away, she worried that she still wasn't saving enough.
"I was stunned by the question," says Thiele, who is general manager of global benefits at Microsoft Corp.
Employees at the Redmond, Wash.-based tech giant, where salaries are high and benefits generous, are hardly typical. But Thiele tells the story to illustrate a point that experts make about millennial workers in general: Despite old stereotypes painting them as entitled and disengaged, millennials, on average, are responsible, even diligent, about saving for retirement. Though some millennials struggle with fear and ignorance about managing their 401(k) accounts, these workers are eager for financial education, experts say.
The 17th annual Transamerica Retirement Survey of Workers, published in August 2016, found that millennial workers started saving at a median age of 22 -- earlier than Generation X or baby-boom workers, who began saving at median ages of 28 and 35, respectively. The survey also found millennials are deferring a median of 7 percent of their income -- barely lower than the 8 percent median for all workers surveyed, despite their relatively lower incomes and long retirement horizons.
Moreover, the survey found, millennials outpaced older generations in the growth of their retirement savings from 2007 to 2016 -- by 244 percent over those nine years, compared to 116 percent for Gen X workers and 96 percent for boomers.
The 2017 Plan Wellness Scorecard, an August 2017 study by Bank of America Merrill Lynch, found that 82 percent of millennial employees enrolled in the 401(k) plans it administers made contributions in 2016 -- well ahead of the rate for Gen X workers (77 percent) and boomers (75 percent).
Getting Started
For all their willingness to save, millennials certainly face financial challenges -- including, for some, relatively low incomes and high student-loan balances. Fear and lack of knowledge about investing also may be barriers, experts and employers say.
For many young workers, getting started is the hard part. Their household budgets usually are slim, and investing for the far-off future is a difficult commitment to make -- especially for young workers unfamiliar with the nuts and bolts of investing, such as understanding the difference between mutual funds and ETFs or evaluating investment fees and rates of return.
Kat Bulger sees the issue from two perspectives. As the resident HR professional in a national home healthcare company's Central California office, part of her job is encouraging the organization's 125 employees to participate in the company 401(k) plan. And at 33, she's squarely in the millennial generation herself.
Bulger says she was excited to start saving after working at smaller companies that lacked retirement plans. "As soon as I started at a company with a 401(k), I signed up as soon as I could," she says.
But Bulger finds that some other millennial workers balk at enrolling out of concern about taking home a smaller paycheck. "For younger employees, [the deduction] seems really large," she says.
Bulger has had some success getting younger workers to participate in their 401(k) plans by emphasizing how small the deduction often is. These workers may make so little that "typically, it's only $20" withheld each pay period, she says. Once they realize it won't affect their daily life, they just leave it and continue to contribute a set percentage of their pay, she says.
Employers can help millennials get over the initial hurdle by adopting an auto-enrollment feature in their 401(k) plans, experts say.
With student loans burdening many millennials, "there's only so many dollars to go around," says Martha Hayward, a vice president for marketing at Boston-based Fidelity Investments, a major provider of employer-sponsored 401(k) plans. To get young workers saving early, she says, "auto-enrollment is crucial."
A new report by investment giant Vanguard, How America Saves 2017, found that the average participation rate in its 401(k) plans with auto enrollment was 90 percent, compared to an average of 81 percent for all plans.
When it comes to designing retirement plans that suit millennial employees, auto enrollment is just the beginning. Other "autopilot" plan features that employers can choose to simplify retirement saving for employees are rapidly gaining popularity. These include automatic contribution increases and the inclusion of "target date" mutual funds that rebalance their investment mixes over time to better fit the likely risk tolerance of account holders as they age.
By 2016, 90 percent of the 401(k) plans that Vanguard administers offered target-date funds and 72 percent of all participants invested in them, according to the firm's 2017 report. In addition, Vanguard reports that 45 percent of the plans it administers have adopted automatic enrollment, up from 27 percent in 2010.
Betterment is among a handful of investment firms that have taken the autopilot idea a step or two further, offering "robo-investing" services to retirement savers. The New York-based company is courting millennials by offering a combination of automated and human advice. In July, the company announced it also will allow account holders to ask questions of a human financial adviser through a secure messaging tool. (Unlike many other robo-advisors, it also offers 401(k) plans to employers.)
The average age of Betterment's customers is 37, says Nick Holeman, a certified financial planner with the company. Holeman believes employers should look for "subtle nudges" to help steer millennials on to a safe path to retirement. Enabling auto-enrollment and setting appropriate default choices in their plans goes a long way in helping them achieve this objective, he says.
Closing the Knowledge Gap
Bulger says a lack of financial knowledge amplifies the fear many of her millennial workers have about retirement saving. "A lot of them don't have a grasp" of financial basics like the power of compounding, Bulger says. "They don't know how the stock market works."
A 2015 study by George Washington University's Global Financial Literacy Excellence Center and PwC found that many millennials know little about money and investing. Only 24 percent of those surveyed demonstrated basic financial knowledge, according to a report on the findings.
The Transamerica survey, meanwhile, suggests millennial workers would like to see their employers come to their aid as far as financial education is concerned: Of those surveyed, 75 percent agreed they "would like to receive more information and advice from my company on how to achieve my retirement goals." Only 55 percent of baby boomers said the same.
One way to keep millennials engaged in planning and saving for retirement is reframing the goal to make it more compelling for a young worker, says Shane Bartling, a senior consultant with Willis Towers Watson in the San Francisco Bay Area. Being young, millennials naturally may see retirement as more theoretical than real, he notes.
"It comes down to making it more tangible," Bartling says. He recommends that employers make the point that saving for retirement also can be seen as saving to become financially independent, free to pursue hobbies or other nonprofessional passions. "It's really just rebranding retirement," he explains. "It's a much more compelling value proposition."
This approach has successfully improved millennial retirement-plan engagement, he says.
Further evidence that millennials are more motivated by the prospect of financial freedom than by simply ceasing to work for a paycheck can be found in Merrill Edge Report, released in May. The study revealed that 63 percent of millennials agreed with the statement, "I am saving to live my desired lifestyle." Only 37 percent agreed with the statement, "I am saving to leave the workforce."
Lack of knowledge isn't the only reason millennials are leery about investing. Many experts link it to a formative experience common among this demographic: As teenagers or young adults from 2007 to 2009, they watched their parents' generation struggle financially, or even fail, during the Great Recession. Some experts say that has shaped how many of them think about money.
"The 2008 recession left an indelible mark on an entire generation," Rosell says. While boomers could trust that living below their means would be enough to build a secure financial future, "that's not necessarily true today," particularly with high levels of student debt among millennials, says Rosell, whose latest book, Keep Climbing: A Millennial's Guide to Financial Planning, aims to engage millennials in financial planning by comparing saving to scaling a mountain.
Holeman agrees. People who lived through the financial crash are "naturally more cautious," he says, adding that "many are still affected by it eight years later."
Among those still affected is Bulger, the millennial HR practitioner in California. "Just as we were becoming adults, that's when it all hit the fan," Bulger says. As a result, "I'm a little paranoid" about finances, she says.
Zoë Fox has a similar attitude. Now a 29-year-old realtor in Philadelphia, Fox remembers a college friend who had to drop out after her parents suffered a foreclosure during the financial crisis. Does that memory affect her philosophy about retirement savings? "Absolutely -- I'm super conservative about money," she says.
Modifying the Match
Employers have another simple, yet powerful method that can help encourage cash-strapped millennials, or employees of any generation, to overcome their investment fears and participate in the 401(k) plan: increase the employer match.
That's what Microsoft did last year, when it began matching half of each participant's contribution, up from half of an employee's first 6 percent of pay deferred. Now, about 90 percent of Microsoft workers participate in the company's 401(k) plan.
Not every company has the cash to contribute as much as Microsoft does to employee retirement savings. Other effective strategies, however, are well within the reach of any organization.
How an employer structures its match also can make a difference, say the authors of the Transamerica report. They recommend that employers encourage employees to save more by matching half of the first 6 percent a worker contributes, for example, rather than the first 3 percent.
Another relatively easy approach, Thiele says, is to tailor communications to different segments of the workforce -- a step that could be particularly effective with millennial workers who have little experience with saving for retirement.
At Microsoft, employees are allocated into 13 "buckets" based on factors such as how -- and how much -- they save, with each "bucket" getting its own stream of communication. That way, millennials who may not be as engaged in their 401(k)s as other demographic groups are able to receive messages that are more tailored to their situation and needs.
Thiele's advice: "If you don't have resources to increase your match, get rid of your old, tired communications campaign."
It's also true that millennials are generally more comfortable with technology than most older workers. Experts, therefore, recommend choosing a plan administrator that offers participants mobile access to their accounts.
The Transamerica survey found 80 percent of millennial workers preferred 401(k) providers that offer mobile access.
At Vanguard, mobile devices now represent 22 percent of all client contacts (compared to 17 percent through telephone calls to a Vanguard representative), as millennials become the workforce's largest generation. The company did not break out figures for mobile access in previous annual reports.
"Millennials are different," says Zane Dalal, executive vice president of Benefit Program Administration, a Los Angeles-based company that manages benefits programs for employers and trade unions. "They're used to doing everything with two thumbs" on a smartphone, he says.
Experts agree that employers are going to need to do a better job recognizing and addressing those differences if they hope to successfully engage millennials in saving for the future.
Zane Dalal is Executive Vice President at Benefit Programs Administration, a third party administrator based in Los Angeles.
This article originally appeared on Human Resource Executive
Benefit Plan Sponsors Need TPAs
Why DIY plan administration is usually not a great idea
A third party administrator isn’t, necessarily, a necessity for every business with a self-insured health plan or a retirement plan, but, for many businesses and business owners, using a TPA can be a cost-effective solution.
When a business owner client is considering whether to use a TPA for a self-insured health plan, for example, the client should consider these three areas:
1. Analytics: Is the employer getting good data on enrollee health care trends?
2. Pharmacy costs: Is the employer doing a good job of containing specialty drug costs?
3. Wellness: Does the employer have a good program for preventing problems, and treating small problems, before small problems turn into big problems?
TPAs may not always have the answers themselves, but they have connections with the experts and vendors that do.
Another factor to keep in mind is whether an employer’s internal systems can handle the administration of a plan, and the tailoring need to meet the needs of each employee.
Going off some ‘one-size-fits-all’ software might initially relieve office stress, but, ultimately, that approach will probably fail to serve the best interests of the business.
A good TPA can customize a plan’s fit. A good TPA can also change the plan as the employer grows and changes, to make sure any employer or employee needs that develop will be taken care of.
A good TPA will also use customizable, adaptable technology, and work to keep the data secure from external threats and data breaches.
Finally, businesses and business owners must consider fiduciary responsibility, which TPAs are uniquely equipped to handle.
Complying with state and federal benefits administration requirements can be time-consuming at best, and the penalties for improper implementation can be hard on an employer’s bottom line. Now, Congress is working on a new round of legislation that threatens to turn everything on its head. Using a TPA is a good way for an employer to handle the uncertainty.
Zane Dalal is Executive Vice President at Benefit Programs Administration, a third party administrator based in Los Angeles.
This article originally appeared on ThinkAdvisor
Why Unions are important! A historical perspective – then and now.
Zane Dalal

For more than a thousand years, as populations migrated from a scant rural existence to congregate in large city centers, there has been the very natural and necessary need to organize trade and commerce. The larger the field of competition the more it became necessary for laborers to band together so their earning power and their individual position in the marketplace allowed them a stable way to provide for themselves and their families. The medieval period flourished with extraordinary ‘guilds’, or confraternities. The idea of student guilds led to the three illustrious universities of Oxford, La Sorbonne and Bologna. The great cathedral builders of the period established themselves as master masons, then freemasons extending a huge mantle of influence long after cathedral building was done. Name a trade and it developed its ‘guild’, then its ‘worshipful company’ and then transitioned into a ‘livery company’. The word ‘company’, in common usage today, is a trade based, labor based term that refers to the organized grouping of a labor force. The remarkable story of apprentice and journeyman is an equally important part of this ancient construct. Leaf through a Summary Plan Description (SPD) of a modern union benefit trust fund and this age-old tradition leaps off the page at you. It is the story of pride in a special skill well executed and well passed on for the next generation. It is the story of communal success. It is the story of burgeoning trade and commerce that drives society, and in its American context it is the living realization of ‘e pluribus unum’.
The rise of the Labor Unions, especially in the United States, was tied strongly to the social need to organize. As the industry changed from household craftsmen to mechanized factories, the market expanded beyond local boundaries. From the multiple factory trades culminating in the great port cities of the Eastern seaboard to the bakers of New York, society was coming to terms with new levers of supply and demand. Regulation was non-existent and many labor related disputes that arose were underscoring specific problems for the first time. I mention the bakers of New York, because it was the landmark Supreme Court Case Lochner v. New York (1905) that is often cited as ‘what not to do’ when trying to decide the merits of a specific labor related case. The final opinion construed the Fourteenth amendment’s ‘due process’ clause to contain a ‘freedom of contract’ right, holding that limits imposed on working hours in any given day violated that right. Justice Oliver Wendel Holmes and Justice John Marshall Harlan’s dissents are shining pieces of jurisprudential history. The bakers of New York, might have relied on weird, 'wee morning hours' to manage their industry, many employees sleeping on the floor in their warm bakeries to be able to facilitate an early start. Quite apart from the unsanitary health concerns, it was not a good model to validate long work hours with almost no regulation. Lochner was controlling case precedent that cut deeply into labor rights and only found partial reversal in the 1937 case West Coast Hotel Co. v. Parrish. The unions that developed in strength from the 1890’s to the 1930’s did so precisely because, left to congress and the courts, a workforce could not be reliably protected.
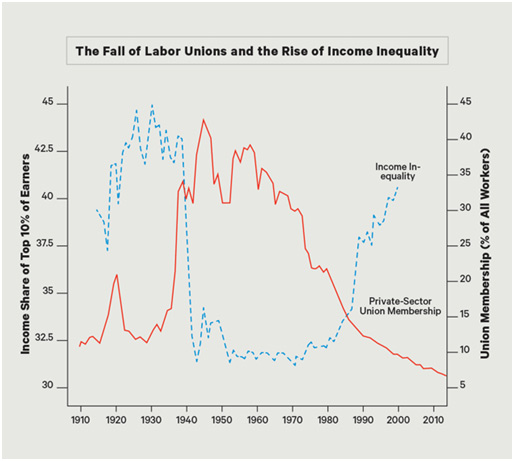
The rise of the Unions and the stability of its members’ earnings allowed the emergence of a middle class in the United States, which in turn drove a factory based, economic machine as never seen before on the planet. The global spread of American influence is deeply rooted in that economic power which allows for a direct and unambiguous link between Union strength and America’s rise as a world super power. The workforce and its cohesive ability to make miracles is the great story of military production during World War II. With war time exigencies over, management expected production to continue at breakneck speed, without the inspiration of a common goal, improved working conditions or pay. The ensuing labor disputes of 1946 which brought many industries to a standstill resulted in The Labor Management Relations Act (1947) or Taft-Hartley as it’s generally known. Passed by congress over President Truman’s veto, it’s another example of a congressional quick fix to problems that were wide ranging and complex. Taft-Hartley was passed primarily for its executive power to force people in protest back to work, than for its equally balanced boards of negotiated governance. Just at a time when unions might have been strengthened, they found themselves curbed by federal law driven by the political and partisan swing in Washington, D.C.
Fifty years ago, almost one third of the American workforce were members of a union. Now the number is closer to one tenth. Income inequality, not only in the United States but in other developed nations across the globe, is a byproduct of a disappearing middle class. Wage earnings for non-union workers have historically always followed the trends indicated and initiated by unions. The benefits arranged by bargained agreements, set the standard for not just the workforce, but for life, family, community and society. The decline of the middle class and the rapid rise of income inequality are directly linked with some of today’s hot button issues such as homelessness, uninsured healthcare, overpopulated prisons, addiction, and the mental health crisis. Two years ago a Pew Research survey conducted in forty-four countries placed inequality as one of the ‘greatest threats to the world.’
We stand at a crucial crossroads. A new, inspired, quick-to-move, upcoming workforce is in play. The millennial group – anyone 35 years of age and below – will be the driving force of a new American age. They have the same natural and instinctive yearning to belong to a group – a club – rich in resources and beneficial to their common goals, just as their forebears from earlier generations. It is time to offer them not what we have, but what they want. A surge in union strength might be more than a rescue of the middle class, it might be a moral imperative.
Zane Dalal is Executive Vice President at Benefit Programs Administration (BPA)
An experienced So. Cal. TPA serving the Taft-Hartley Industry since 1948
The Future of the ACA

Intro
For more than 70 years, Benefit Programs Administration (BPA) has been entrusted with the administration of benefits plans for American workers through single- or multi-employer trust funds. As the health care sector has grown and changed over the last seven decades, so has BPA. Now, Congress is contemplating the second major health care overhaul in a decade. Keep reading for a high-level explanation of the current state of health care and where health care legislation may be headed.
The Affordable Care Act (ACA) is a federal health care bill that passed in 2010. The bill was the largest overhaul of the health care industry since the creation of Medicare and Medicaid in the 1960s. The ACA expanded insurance coverage and mandated that every American must have health insurance. Provisions in the ACA included expanded mental health coverage and outlined “essential benefits” that all insurance companies must cover.
Despite the entire ACA structure being dependent upon employer-centric insurance coverage, the law did not address the specific needs of the Taft-Hartley fund model. Typically, before and after initial passage of a law there is a customary review period and exchange of briefs and papers before statutes are enforced. For the ACA, this period led to considerable back and forth between the industry and Washington, D.C., ending in a stop gap resolution that effectively allowed each individual fund under the Taft-Hartley model to operate as if it was a health care exchange under ACA. Rules for “grandfathered” status were introduced to allow certain funds time to transition to new benefit packages.
Current and future status of health care
Currently, the ACA is the health care law of the land. New legislation, the American Health Care Act (AHCA), has been proposed to replace the ACA. The AHCA has passed in the House but not the Senate. If and when the bill passes in the Senate, the two versions of the bill would need to be reconciled before going to the president’s desk.
The crafters of the AHCA consider it a relief on undue taxation. Opponents of the new legislation say that the bill’s sweeping, deep cuts do not address health care, deny the benefits of recently acquired health insurance and create consequential problems from which it may be difficult to recover. Both sides are rightly concerned by passing measures in haste for partisan or procedural reasons that will affect the lives of millions of Americans.
Conclusion
The complexities of health care ensure that whatever the changes, tensions will run high as the country adapts to a second round of federally mandated provisions. Just as with the ACA, state legislators may opt in or out of various provisions as they choose how to serve their constituents. A changing landscape is not new to the Taft-Hartley industry and the professionals that serve it. Benefit Programs Administration stands ready, as it has done for almost 70 years, to partner with trustees, professionals and participants to make sure that understanding, compliance and implementation is a smooth and seamless process.
PLANSPONSOR: A Closer Look at Plan Health

By Javier SimonAs defined benefit (DB) plans shrink in number and the future of Social Security benefits dips further into uncertainty, defined contribution (DC) plans and individual retirement accounts (IRAs) are becoming the primary tools driving America’s retirement security.
However, many Americans are behind on retirement readiness. More than half (52%) of households are at risk of not being able to maintain their standard of living in retirement, according to a recent study by Prudential and the Center for Retirement Research at Boston College (CRR).
And with a heightened scrutiny on fees and fiduciary responsibility, it’s becoming increasingly important for plan sponsors to ensure their participants’ retirement readiness and maintain a healthy plan.
Sean McLaughlin, senior vice president, head of client relations and business development, Prudential Retirement, tells PLANSPONSOR that a major component to any healthy plan is “the right plan design for your participants.”
Features such as auto-enrollment have been among the biggest drivers of higher participation, according to Wells Fargo’s study “Driving Plan Health 2016.” Still, the Plan Sponsor Council of America (PSCA) found that the most common auto-enrollment salary deferral rate is 3% of pay. “We recommend closer to 6%,” says McLaughlin.
While some sponsors may fear this would reduce participation rates, volumes of evidence suggests otherwise.
Wells Fargo’s data indicates that plans which have auto-enrolled participants at a deferral rate of 6% averaged 87% participation rates. The figure is 83% for those that auto-enrolled at 3%. The firm also notes that opt-out rates “do not vary substantially from lower to higher default deferral rates,” and that plans with lower default deferral rates naturally have overall lower average deferral rates.
NEXT: Plan design and plan health
Furthermore, the PSCA found only 65% of plans with auto-enrollment utilize auto-escalation. McLaughlin suggests auto-escalation of 1% annually up to 10%, “or more if the employee population can save more.”
Auto features are so important to a healthy plan because otherwise a whole lot of people will never take the necessary action to enroll themselves, even if they like the idea of saving, warns Zane Dalal, executive vice president at Benefit Programs Administration (BPA). “Let’s say you get into a 401(k) in your 20s, and by the time you’re ready to retire, you can have $1 million. If you were not clear about this in your 20s and decide to start contributing in your 30s, you’d only have about $630,000. It’s a huge disadvantage.”
McLaughlin suggests plan sponsors “auto-enroll until people give up and they’re in the plan. Do it on an annual basis, reenrolling the entire eligible population.”
A company match can also go a long way, even without auto-enrollment. The Wells Fargo’s data indicates that for plans without auto-enrollment, the average participation rates were higher for those with the larger matches. Plans with matches up to 3% averaged 48.7% participation. Plans with matches between 6% and 9% averaged 64.6% participation.
But regardless of how much money employees defer, what matters most is where that money goes.
NEXT: choosing the right investments
Alleged excessive fees have been central to plenty of the current litigation surrounding the DC space. Thus, to have a healthy plan, sponsors have to maintain a cautious eye when selecting investments for their qualified default invest alternatives (QDIAs), and understand the different share classes available across the entire core menu.
This decision can and should rely heavily on employee demographics. Target-date funds (TDFs) and managed accounts offer the advantage of letting participants hand over investment management to professionals. And while TDFs currently dominate the DC space, they can vary widely based on provider.
Prudential’s paper notes that “sponsors should consider how well a target-date fund’s characteristics align with the demographics of the plan. The glide path design should address the right risks at the right time—target date funds need to be aggressive enough to address longevity challenges while not over-exposing participants to market risk near retirement.”
And while basic demographics tell a sponsor a lot about participants’ risk tolerance, other factors should also be used to dig deeper. The job itself can play a significant role in how an employee saves.
“Different industries have different expected return and profit levels, which makes more or less money available to invest in a retirement program for employees,” says McLaughlin. “Industry matters a lot, and it has to be factored into plan design. Sponsors need to speak specifically with advisers, providers and stakeholders to discuss their needs as an organization and where they are in their lifecycle, whether it be a start up with limited cash or a large and very successful firm.”
This, along with fund performance and costs, are some of the main points to consider when selecting a fund lineup. Choosing the right options could not only attract and retain the best talent, but also provide the right amount of turnover.
NEXT: Helping participants retire on time
“One of the challenges that has been much more common since the financial crisis has been workers not retiring at a ‘normal’ retirement age, and sticking out longer than employers may have planned,” explains McLaughlin. Research sponsored by Prudential notes that a one-year delay in retirement may result in incremental workforce costs of 1% to 1.5% annually.
McLaughlin suggests that one way to address this issue, along with the fear among participants of outliving their assets, is to incorporate an in-plan guaranteed lifetime income (GLI) product.
He alludes that even if a participant has enough assets to feel retirement ready by the time he reaches that milestone, the drawdown phase poses another challenge. “How does he take that money as income? Most folks don’t have expertise around that. So, having an in-plan income option is really helpful.”
Prudential also notes that GLI may serve as a backdrop for participants in the event that a severe market downturn impedes retirement readiness. One of the firm’s recent surveys finds that 53% of financial executives believe participants will engage in less risky behavior—like getting out of investments at the wrong time—if they are invested in some kind of GLI product.
“The biggest mistake you can make is jumping in and out of the market,” says BPA’s Dalal. “It’s the biggest killer in the investment world.”
Choosing the best fund lineup would help plan sponsors meet their fiduciary responsibilities and comply with various regulators in the DC space. In this realm, it’s also important to leverage support from all parties involved in the plan.
“Consultative regulatory services can help plan sponsors navigate the complexity of having a DC plan,” McLaughlin concludes. “They can look at plan documents, plan design and all of the different elements that tie back to regulation before making a set of recommendations.”
But even solid plan design and a strong investment lineup will fail to reach the plans’ full potential if participants aren’t utilizing the plan properly. Education is key to driving engagement. Many tools can boost engagement and help participants think of retirement as a piece to overall financial wellness. And these can be integrated with the existing benefits package to control costs.
This article originally appeared in PLANSPONSOR.
PLANSPONSOR: Multiemployer Plans Have Hope and a Future

By Rebecca MooreWe’ve all seen the headlines: The Pension Benefit Guaranty Corporation (PBGC) multiemployer plan program is running out of money because it is helping so many plans, and a number of multiemployer plans have asked the Treasury for permission to reduce benefits under the Multiemployer Pension Reform Act (MPRA).
But, according to Zane Dalal, executive vice president of Benefit Programs Administration (BPA), who is based in Los Angeles, the industry needs to take a balanced view.
First of all, the multiemployer (or Taft-Hartley) plan market is large. Dalal notes that as of 2014, there were 2,671 multiemployer plans—1,403 defined benefit (DB) and 1,268 defined contribution (DC). Taft-Hartley plans not only include a DB plan, but many times also a health plan, and Dalal says, in many cases a DC plan is offered as a supplement to the DB plan, not as a replacement.
In 2014, there were 15,280,000 participants and beneficiaries in multiemployer plans—10,703,000 in DB and 4,577,000 in DC. Also, $703 billion in assets were held by multiemployer plans—$500 billion in DB and $203 billion in DC.
David Brenner, national director of multiemployer consulting with Segal Consulting, who is based in Boston, says the reason there isn't more current information is it comes from Form 5500 data. “By the time we get information, it is 12 to 18 months out of date,” he says.
SVP and actuary Diane Gleave with Segal Consulting, who is based in New York City, says the number of plans can decline because some plans terminate and some plans merge. But, Taft-Hartley plans are not going the way of the dinosaur. “We are seeing some new plans being created in some instances. For example, pieces of plans can be transferred out of a current plan to a new plan, subject to regulatory requirements that have to be satisfied,” she notes.
Brenner adds that new plans are being created in the building and construction industries.
And most plans are doing well. The latest Survey of Plans’ Zone Status from Segal Consulting shows that a majority of multiemployer plans are still in the green zone. The survey found 64% of plans are in the green zone, while the percentage of plans in the yellow zone and red zone remained stable at 11% and 25%, respectively. These numbers are virtually unchanged compared to data for the previous 12-month period.
Gleave says many plans are even thriving, so multiemployer plans’ situation is not as dire as reports indicate, though she concedes there are a significant number of participants in distressed plans.
“The majority of plans we work with are in the yellow or green zone, and funding is improving,” Brenner says. “The boards of trustees for these plans look at the big picture and look at their world and have begun to ask questions about alternatives to what they are doing. The majority of plans out there are stable and well-run and have tremendous futures. They are challenged with the legacy of bad market returns and for the most part are stepping up to deal with it. They are working with investment consultants to see if there are new and different ways to invest; working with actuaries and consultants to think about costs; considering subsidies they provide now whether to reduce them; and whether they should shift from only a DB plan to that plus a companion DC plan.”
NEXT: Multiemployer plan struggles
As with any retirement plan type, multiemployer plans are subject to market volatility. According to a report from Horizon Actuarial Services, LLC, at the height of the financial collapse in 2008, the median investment return for multiemployer DB plans was -23.5%. However, the median annualized return was about 5.6% over the 10-year period from 2005 through 2014, and the 2014 median investment return was 6.3%.
According to Dalal, there are two other struggles multiemployer plans face. One is a change in the workforce. “Millennials’ representation in this old, union model is not as good as it should be,” he notes. In addition, the Pension Protection Act’s multiemployer plan provisions were meant to create more transparency and more policing. “But, when the government is involved, good people doing the right thing have a load of reporting placed on them. Instead of making things transparent, the PPA created an extra costly burden coming out of retirement funds,” Dalal says.
“The Taft-Hartley model is not dissimilar to Social Security. The idea of having enough actives contributing what will be required by retirees is not something we have control of,” Dalal adds. And, he notes that the whole populous is living longer—the amount retirees will continue to collect is something multiemployer plans need to consider.
For Brenner and Gleave, it’s all about the economy. Brenner says for some plans in critical and declining status, it’s not that their being badly managed or making bad investment decisions, it’s about the economy. He notes that many construction companies in the Midwest haven’t recovered from a downturn in the economy. Many have not seen a resurgence in the particular industries in which they work. Other industries have fled the United States, and for others, deregulation, such as for teamster plans, have hurt them. He explains that back in the 1980s, the trucking industry was highly regulated. The government began the process of deregulating, which introduced much more competition and growth of a non-union trucking sector, which has penalized historic, legacy trucking firms.
"It's hardly surprising that plans covering workers in hard-hit industries, like coal, are facing challenges," Brenner adds.
NEXT: The future for multiemployer plans
For plans going forward, Gleave says there are three levers: asset allocation; plan management of what benefits are being provided and the costs and how to manage that; and a look at plan design provisions to see if a shared-risk design is better able to withstand volatility.
She explains that shared risk is a broad category with a lot of different options. It could be something as simple as if the plan meets certain targets, participants will have a benefit accrual of ‘x’ dollars, but if not, they will have an accrual of ‘y’ dollars. On the other extreme is truly variable plan design; benefits that have been accrued can vary based on certain metrics.
Gleave notes that the National Coordinating Committee for Multiemployer Plans (NCCMP) has proposed a composite plan, viewed as shared-risk design that could be used if enacted. It is a concept of shared risk between the plan, participants and employer members.
Dalal says the multiemployer plan market has solutions to take care of administration and investments, new rules and legal compliance, research on demographics, participant services, and cybersecurity. “We’re already there, unions just need to be willing to change and add components such as health savings accounts (HSAs), health reimbursement arrangements (HRAs), multiemployer welfare arrangements (MEWAs), and financial wellness. The idea is to get people to come in to a rich, resource-ready club.
Unions need to tweak plans so Millennials say ‘That’s a good deal to me.’ “For some reason, in the modern world the word ‘union’ seems to have a negative connotation. It’s up to unions to change that; to show they are not adversarial to employers, but are about participants having resources to do things for themselves. Millennials are people that will need this and expect it for a long retirement,” Dalal says.
“Millions will retire well with these plans, and the plans are not going away. The industry doesn’t want to lose sight of that,” Brenner concludes.
This article originally appeared in PLANSPONSOR.
We’ll See You at the IFEBP Conference this October

What happens in Vegas ... will be brought back to BPA HQ to better serve you! This October, BPA will host an exhibit at the 63rd annual Conference of the International Foundation of Employee Benefit Plans (IFEBP) at the Mandalay Bay Convention Center in Las Vegas, Nevada, and we’d love to see you there.
In a year when significant changes to our health care system and retirement structure are all but guaranteed, it’s never been so important to stay abreast of industry trends and connected with our colleagues. The IFEBP offers more than 100 sessions designed to give our experts a deeper understanding of pension strategy, plan design options, risks, legislation and security, so that we can find effective solutions and bring hard-dollar cost savings to our clients.
We look forward to congregating with more than 5,000 of our colleagues and introducing new insights into our collaborative headquarters. Our team has been attending the IFEBP’s annual conference for many years to provide information about BPA’s industry-leading offerings. So if you’re planning to attend, please stop by our exhibitor’s booth.
What: Conference of the International Foundation of Employee Benefit Plans (IFEBP)
Where: 3950 S Las Vegas Blvd, Las Vegas, NV 89119
When: October 22-25, 2017
Movin’ On Up
BPA has a new address!
Our new office space on the fifth floor of 1200 Wilshire Boulevard has expansive windows overlooking downtown Los Angeles, designed to flood the spacious common areas with natural light. The modern, open layout encourages the BPA team to communicate and collaborate, which has given a significant boost to teamwork and morale. Staff and clients alike love the new look.
This strategic move is reflective of BPA’s dynamic new direction, and positions us to continue to provide excellent service to our clients and promotes a new, integrated and vibrant office for our personnel.
The freshly renovated building is located in the central downtown Los Angeles area, putting us at the center of a premier business hotspot. Our clients appreciate the conveniences and take advantage of our ample, meticulously designed meeting spaces to host quarterly and annual meetings.
Please update your address books, and don’t hesitate to pay us a visit in our brand new space!
Welcoming Teamsters Local 572 to BPA

Benefit Programs Administration is proud to announce a new partnership with the Teamsters Local 572. We look forward to a close and long lasting relationship as we serve the participants of the Teamsters Multi-Benefit Trust & Local Union No. 572 Retirement Benefit Plan.
Chartered by the International Brotherhood of Teamsters in 1937, Teamsters 572 is currently one of the largest locals in the state of California. The union currently represents more than 150 different employers in a wide array of industries including bakery, graphic communications, retail, soft drink, transportation, grocery and specialty businesses.
BPA will administer both the Teamsters’ Local Union No. 572 Retirement Benefit Plan, a defined contribution plan originally adopted in Sept. 1994; and the Multi-Benefit Trust, a multi-employer plan formed under a collective bargaining agreement with participating employers and the International Brotherhood of Teamsters located within the Jurisdiction of Joint Council of Teamsters No. 42.